
Ovarian Cancer
What is Ovarian Cancer?
Ovarian cancer begins in the ovaries, fallopian tubes, or the peritoneum (lining of the abdominal cavity). It is often called the "silent killer" because early symptoms are vague and easily mistaken for digestive or urinary problems. Put simply, ovarian cancer happens when abnormal cells in or near the ovaries grow uncontrollably. If not detected early, these cancerous cells can spread to other parts of the body.
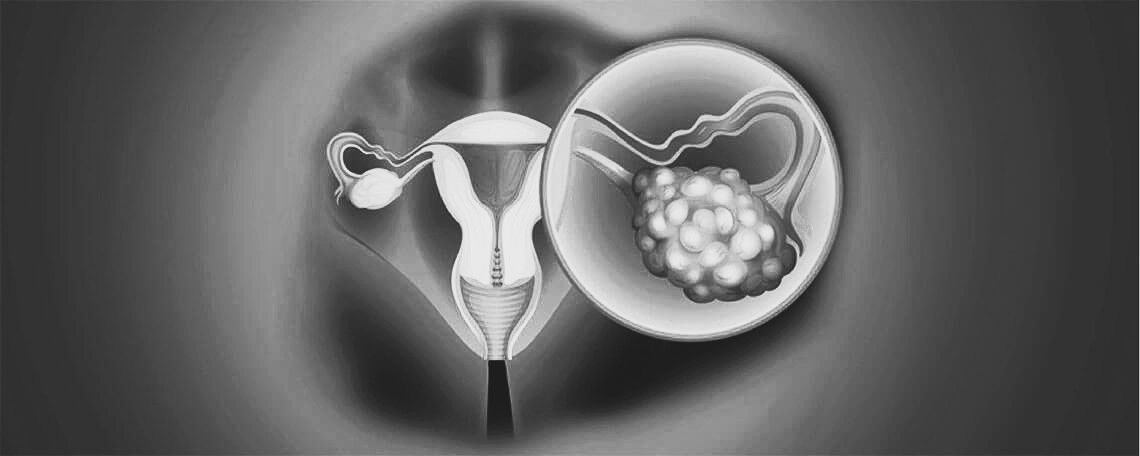
Ovarian Cancer Types
Epithelial Ovarian Cancer
•The most common type, which arises in the surface layer of the ovary. Usually diagnosed at advanced stages and responds well to surgery and chemotherapy.
Germ Cell Tumors
•Uncommon and most often seen in younger women. These tumors occur from egg-producing cells and have a very high cure rate when treated with surgery and chemotherapy.
Stromal Tumors
•Develop in hormone-producing cells of the ovary. Usually diagnosed early and can secrete hormones such as estrogen or testosterone, both directing diagnosis and treatment.
Ovarian Cancer Symptoms
- •Continuous abdominal bloating or swelling that doesn’t go away is a common early symptom due to fluid buildup or tumor growth.
What’s Notable
The most common type is epithelial ovarian cancer, which includes subtypes like serous and mucinous carcinoma.
Less common are stromal tumors and germ cell tumors, which are more likely to be diagnosed early and often affect younger women.
More common in urban Indian women due to lifestyle and reproductive factors.
When to Seek Help
You should see a doctor if you have persistent symptoms like bloating, pelvic or abdominal pain, feeling full quickly, urinary changes, or unusual vaginal bleeding lasting more than two weeks. Early medical evaluation is important for timely diagnosis and treatment.
Ovarian Cancer Causes & Risk Factors
Older Age
Risk increases with age, especially after 50 years.
Inherited Gene Mutations
Genes like BRCA1, BRCA2, and others increase risk.
Family History
Having close relatives with ovarian or breast cancer raises risk.
Hormone Replacement Therapy
Use after menopause may slightly increase risk.
Obesity
Being overweight can raise the chance of developing ovarian cancer.
Reproductive History
Never having been pregnant or having first pregnancy late.
Menstruation Factors
Early periods or late menopause may raise risk.
Ovarian Cancer Diagnosis
Initial Symptoms & Check-up
Step 1: Initial Symptoms & Check-up
Symptoms: Bloating, pelvic pain, urinary changes Physician performs physical exam and pelvic imaging.
Ovarian Cancer Treatment
Chemotherapy
What it does:
Kills rapidly dividing cancer cells in the body.
Common drugs:
Carboplatin, Paclitaxel
Side effects:
Fatigue, nausea, low blood counts, neuropathy
Targeted Therapy
What it does :
Inhibits specific cancer pathways
Common drugs:
Bevacizumab, PARP inhibitors (olaparib)
Side effects:
Hypertension, fatigue, blood abnormalities
Immunotherapy
What it does:
Stimulates the immune system against cancer
Treated for:
Experimental or clinical trial settings
Common drugs:
Checkpoint inhibitors
Side effects:
Inflammation, fatigue, thyroid dysfunction
Management & Prevention
Rest and Healing
•After ovarian cancer surgery, rest for several weeks is essential to allow your body to heal.
Gradual Activity
•Start with gentle walking and light exercises as advised by your doctor to rebuild strength.
Nutrition
•Eat a balanced diet to support recovery and maintain energy.
Symptom Monitoring
•Regular follow-ups help manage side effects and monitor your health.
Ovarian Cancer Types
Epithelial Ovarian Cancer
•The most common type, which arises in the surface layer of the ovary. Usually diagnosed at advanced stages and responds well to surgery and chemotherapy.
Germ Cell Tumors
•Uncommon and most often seen in younger women. These tumors occur from egg-producing cells and have a very high cure rate when treated with surgery and chemotherapy.
Stromal Tumors
•Develop in hormone-producing cells of the ovary. Usually diagnosed early and can secrete hormones such as estrogen or testosterone, both directing diagnosis and treatment.
Ovarian Cancer Symptoms
- •Continuous abdominal bloating or swelling that doesn’t go away is a common early symptom due to fluid buildup or tumor growth.
What’s Notable
The most common type is epithelial ovarian cancer, which includes subtypes like serous and mucinous carcinoma.
Less common are stromal tumors and germ cell tumors, which are more likely to be diagnosed early and often affect younger women.
More common in urban Indian women due to lifestyle and reproductive factors.
When to Seek Help
You should see a doctor if you have persistent symptoms like bloating, pelvic or abdominal pain, feeling full quickly, urinary changes, or unusual vaginal bleeding lasting more than two weeks. Early medical evaluation is important for timely diagnosis and treatment.
Ovarian Cancer Causes & Risk Factors
Older Age
Risk increases with age, especially after 50 years.
Inherited Gene Mutations
Genes like BRCA1, BRCA2, and others increase risk.
Family History
Having close relatives with ovarian or breast cancer raises risk.
Hormone Replacement Therapy
Use after menopause may slightly increase risk.
Obesity
Being overweight can raise the chance of developing ovarian cancer.
Reproductive History
Never having been pregnant or having first pregnancy late.
Menstruation Factors
Early periods or late menopause may raise risk.
Ovarian Cancer Diagnosis
Initial Symptoms & Check-up
Step 1: Initial Symptoms & Check-up
Symptoms: Bloating, pelvic pain, urinary changes Physician performs physical exam and pelvic imaging.
Ovarian Cancer Treatment
Chemotherapy
What it does:
Kills rapidly dividing cancer cells in the body.
Common drugs:
Carboplatin, Paclitaxel
Side effects:
Fatigue, nausea, low blood counts, neuropathy
Targeted Therapy
What it does :
Inhibits specific cancer pathways
Common drugs:
Bevacizumab, PARP inhibitors (olaparib)
Side effects:
Hypertension, fatigue, blood abnormalities
Immunotherapy
What it does:
Stimulates the immune system against cancer
Treated for:
Experimental or clinical trial settings
Common drugs:
Checkpoint inhibitors
Side effects:
Inflammation, fatigue, thyroid dysfunction
Management & Prevention
Rest and Healing
•After ovarian cancer surgery, rest for several weeks is essential to allow your body to heal.
Gradual Activity
•Start with gentle walking and light exercises as advised by your doctor to rebuild strength.
Nutrition
•Eat a balanced diet to support recovery and maintain energy.
Symptom Monitoring
•Regular follow-ups help manage side effects and monitor your health.
Why Choose Everhope Ovarian Cancer?
At Everhope Oncology, we understand that ovarian cancer is more than a diagnosis; it’s a deeply personal journey. With our compassionate care, expert guidance, and innovative treatments, we commit to supporting you every step of the way, offering strength, hope, and healing through your path to recovery.
5th
leading cause of cancer death among women globally.
3M
New cases were reported worldwide.
2M
Deaths were reported worldwide.
Explore Our Latest Updates

FAQs on Ovarian Cancer
No question is too small when it comes to your care
Find a Centre Near You
Gurgaon EBD 65
EBD 65, Sector 65, Golf Course Extension Road, Gurgaon
