Breast Cancer in Pregnancy: What It Means for You and Your Baby

Pregnancy affects your body in ways you can feel, and in ways you’re still noticing the emotional and physical changes. There is often a lot happening at once. It’s a time of planning, adjusting, and preparing for what’s ahead.
But when medical uncertainty comes up during this experience, it can naturally feel like a great deal to process at once.
Care during pregnancy, however, is planned carefully and individually. Specialists consider both your health and your baby’s development at every step.
In this guide, we’ll explain what a breast cancer diagnosis during pregnancy means and how you can safely prioritise your well-being and your baby’s development.
Understanding breast cancer in pregnancy
Your body is currently supporting growth for your baby and undergoing massive hormonal shifts to support you both. Occasionally, those same signals that tell your breasts to prepare for breastfeeding can encourage cancer cells to grow.
It is important to understand that breast cancer during pregnancy doesn’t mean you have to choose between your health and your baby.
With a multidisciplinary team, including your obstetrician and an oncologist, you can navigate a path that prioritises both lives.
What is pregnancy associated breast cancer?
Breast cancer during pregnancy is called pregnancy-associated breast cancer (PABC). It refers to any breast cancer diagnosed during pregnancy or within the first year after giving birth.
Women are now choosing to have children later in life, and breast cancer rates in younger women are slightly rising as well. So we’re now seeing a bit more intersection between these two.
It’s still pretty rare, only occurring in about 15-35 in every 100,000 pregnancies. It is, however, the most common type of cancer found during gestation.
One of the biggest hurdles with breast cancer and pregnancy is the masking effect. Because your breasts naturally become denser, heavier, and sometimes lumpier during pregnancy, it’s easy for a small tumour to hide.
This is why it’s so important to trust your intuition. If a lump in breast feels different or doesn't go away, it's always worth a check.
Most common type of breast cancer in pregnancy
If you are looking at a pathology report, you might see the term Invasive Ductal Carcinoma (IDC), the most common breast cancer in pregnancy. It’s the same "standard" type of breast cancer seen in non-pregnant women.
However, the biology of these tumours tends to be a bit more aggressive in the pregnant population.
The main molecular subtypes of breast cancer that you may see in your pathology report include:
| Subtype | Defined by | What it means |
|---|---|---|
| Hormone receptor–positive (HR+) | ER+ and/or PR+ | Cancer grows in response to estrogen or progesterone. Often responds to hormone therapy. |
| HER2-positive | HER2 protein overexpression | Faster-growing cancer, but treatable with targeted HER2 drugs. |
| Triple-negative breast cancer (TNBC) | ER-, PR-, HER2- | Lacks all three receptors; more aggressive and fewer targeted treatment options. |
Even though these types sound aggressive, knowing exactly what they are allows your team to use the most effective tools to treat them.
Pregnancy and breast cancer risk: What you should know
The link between breast cancer risk and pregnancy is a bit paradoxical. For instance:
The long-term protection
Pregnancy reduces risk of breast cancer in the long run. When you carry a baby to at least 34 weeks, your breast cells undergo terminal differentiation. Essentially, they mature and become more resistant to becoming cancerous later in life.
You may also be wondering about pregnancy after breast cancer. In many cases, a future pregnancy is possible with careful planning and guidance from an oncology doctor.
The short-term window
In the years immediately following childbirth, there is a temporary increase in breast cancer risk. This is because the process of the breast shrinking back to its normal size (involution) involves inflammation and tissue remodelling. This can sometimes cause a stray cancer cell to grow.
This is why staying vigilant about breast cancer after pregnancy is just as important as during the pregnancy itself.
Breast cancer during pregnancy symptoms
Recognising breast cancer symptoms during pregnancy can be challenging because your body is already changing so much. What you may see as tenderness or lumpy milk ducts can be specific warning signs:
- •A firm, painless lump:This is the most common sign. Unlike a clogged milk duct, this lump won't go away with massage or warm compresses.
- •Skin changes:Look for redness, thickening, or pitting of the skin (it might look like the skin of an orange).
- •Nipple changes:A nipple that suddenly pulls inward or unusual discharge (especially with blood).
- •Inflammation:If your breast looks very red, feels hot, or is swelling rapidly, it could be an infection. But if antibiotics don't fix it within a few days, it’s worth consulting an expert for this.
Staying aware of breast cancer after pregnancy symptoms is equally important, especially if your breast anatomy continues to change even after delivery or breastfeeding has ended.
Diagnosis of breast cancer in pregnancy
You may be worried about the baby’s safety with tests, but management of breast cancer in pregnancy begins with safe imaging. If you or your pathologist finds something suspicious, the next step is getting a breast cancer diagnosis done:
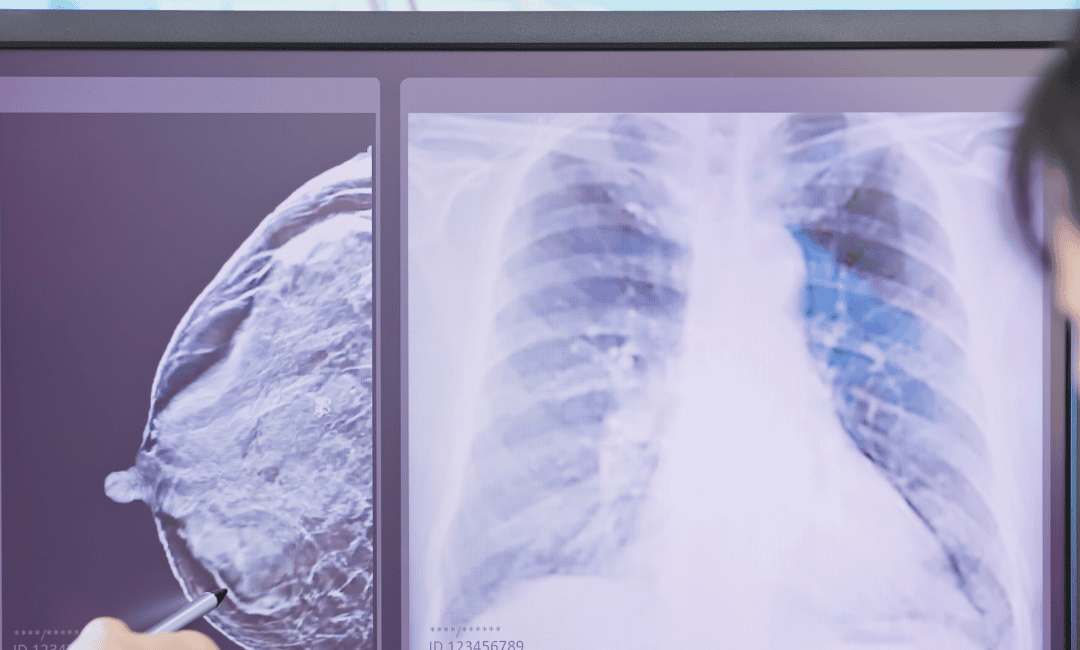
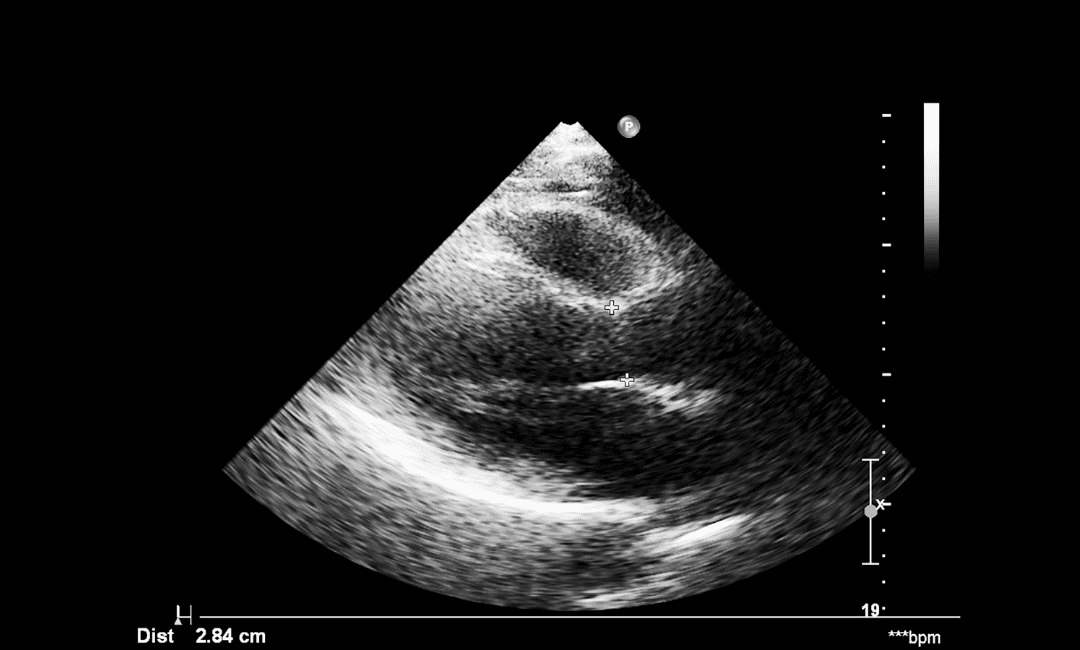
- •Ultrasound:This is the first safe step. It uses sound waves, not radiation, so it’s considered safe for the baby.
- •Mammogram:If needed, you can have a mammogram. Your pathologist will likely use a lead shield over your belly to ensure the baby is not exposed to radiation.
- •Biopsy:A core needle biopsy is safe at any stage of pregnancy. It uses local anaesthetics and provides the definitive answer needed to create a treatment plan.
To note, pathologists usually avoid contrast MRIs during pregnancy for cancer treatment, as the dye can cross the placenta.
Management of breast cancer in pregnancy
The most important thing here is that you can receive high-quality care while pregnant. There are very clear breast cancer in pregnancy guidelines that oncologists worldwide follow to protect both mom and baby.
Surgery
Surgery is generally safe during all trimesters after breast cancer screening. Whether you need a lumpectomy or a mastectomy, modern anaesthesia is very safe for the baby.
If you are in your second or third trimester, surgery is also often the first step.
Chemotherapy
It might sound terrifying to think about chemotherapy while pregnant, but after the first trimester (once the baby’s organs are fully formed), certain types of chemotherapy are remarkably safe.
The placenta acts as a bit of a filter, and studies show that babies exposed to chemo in the second and third trimesters hit their developmental milestones just like any other child.
What is postponed?
According to the breast cancer in pregnancy guidelines, certain things are usually delayed until after the baby is born:
- •Radiation:This is avoided because radiation can scatter toward the womb.
- •Hormone Therapy (Tamoxifen):This can interfere with the baby's development.
- •Targeted Therapies (Herceptin):These can affect the amniotic fluid.
Does breast cancer affect pregnancy?
The cancer itself doesn't usually harm the baby, and it’s very rare for cancer cells to pass to the fetus.
The main goal of the management of breast cancer in pregnancy is simply to ensure the mother is healthy enough to carry the baby to term.
Looking ahead after diagnosis
Finding out you have breast cancer in pregnancy is a heavy weight to carry, but it is not a weight you carry alone. Being pregnant doesn't make the cancer unbeatable, and being treated doesn't mean you can't have a healthy, happy baby.
With early detection and a personalised approach to breast cancer treatment during pregnancy, it’s now possible to treat the mother effectively while the baby continues to thrive. If you have noticed any breast cancer during pregnancy symptoms, do not wait. Most women go on to have healthy babies and successful recoveries after treatment.
FAQs
Related Blogs