Sézary Syndrome: Symptoms, Diagnosis Process & Treatment

Have you been dealing with unbearable itching and red skin for months? Lotions don't help. Your skin feels constantly inflamed. Perhaps you've noticed unusual tiredness or swollen lymph nodes in neck that won't go away.
When dermatologists mention “Sézary syndrome”, the unfamiliar term might leave you confused and frightened. What exactly is this condition? Is it serious? Can it be treated? Sézary syndrome is rare, and you probably haven't heard of it before. That's completely normal. Understanding what you're facing helps reduce fear and guides you toward appropriate care. You deserve clear, honest answers during this difficult time.
What is Sézary syndrome?
Sézary syndrome definition describes a rare, aggressive form of cutaneous T-cell lymphoma affecting your skin, blood, and lymph nodes simultaneously.
The condition is named after French dermatologist Albert Sézary who first described it in 1938. It's one of the more advanced types of cancer in the lymphoma family.
Think of it this way: your immune system contains T-cells that normally protect you from infections. In Sézary syndrome, these T-cells become cancerous. They multiply uncontrollably. What is Sézary syndrome in practical terms? It's a blood cancer that primarily shows up in your skin. Nearly all of your body's skin becomes red and inflamed (called erythroderma), and abnormal T-cells circulate throughout your bloodstream.
How common is Sézary syndrome?
Understanding the rarity of Sézary syndrome helps put your diagnosis in perspective.
According to research, Sézary syndrome is extremely rare, representing approximately 3% of all cutaneous T-cell lymphomas.
Globally, Sézary syndrome affects approximately 0.1 per million people annually. In India, with our population of 1.4 billion, that means roughly 100-150 new cases each year across the entire country.
Who develops Sézary syndrome
The condition most commonly affects people over 60 years old. Men develop it slightly more frequently than women, with a ratio of about 2:1. It's extremely rare in children and young adults.
What do the Sézary syndrome symptoms look like
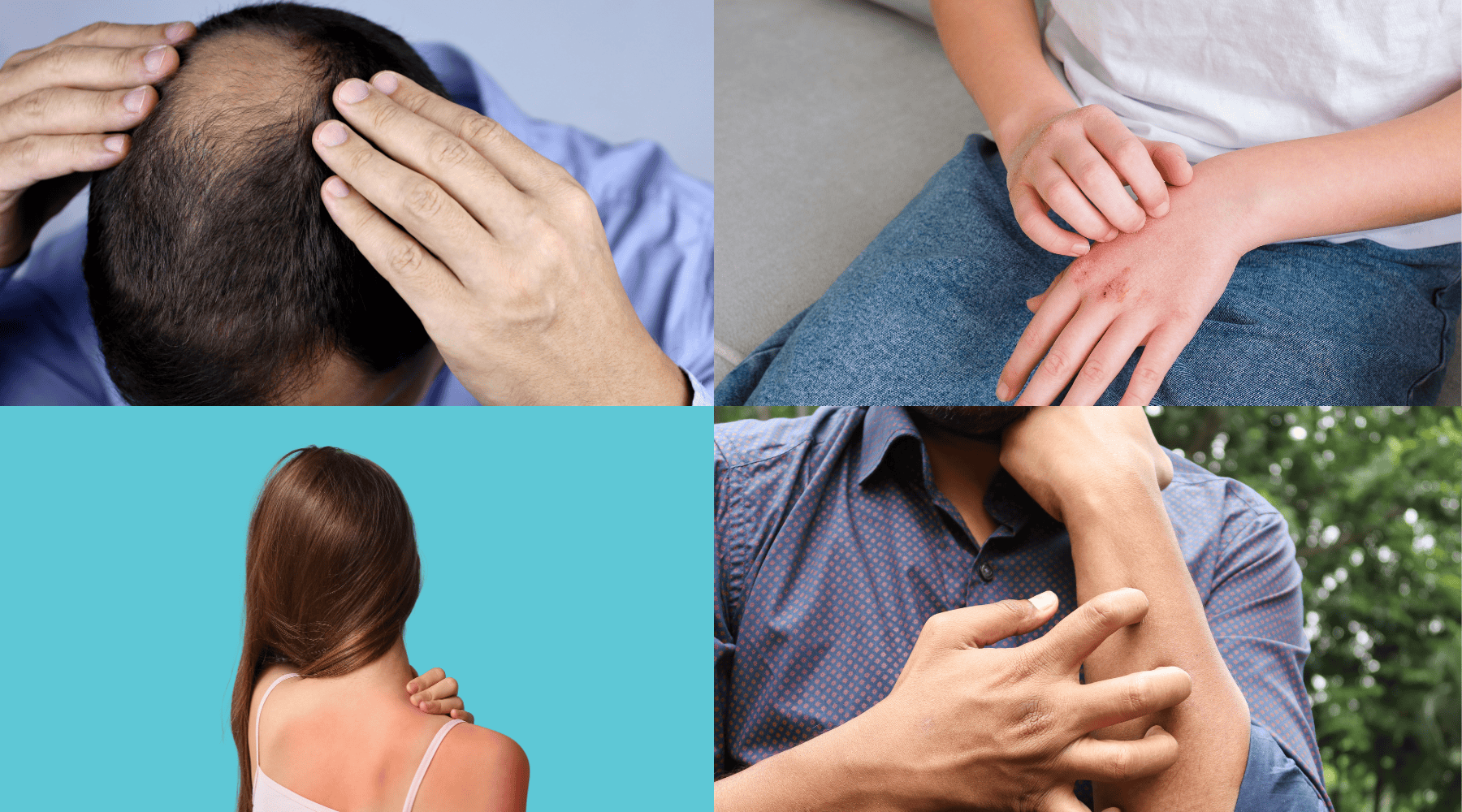
Recognising Sézary syndrome symptoms helps you understand what changes in your body mean and when to seek specialised evaluation. Skin manifestations (present in virtually all patients):
- •Widespreadredness covering 80% or more of body surface (erythroderma)
- •Intense, unbearable itching that disrupts sleep and daily activities
- •Dry, scaling skin that sheds constantly
- •Thickenedskin on palms and soles
- •Hairloss (alopecia) as skin involvement progresses
- •Nailchanges including thickening, ridging, or loss
Blood involvement shows through:
- •Extremefatigue and weakness (cancer fatigue is profound)
- •Increasedsusceptibility to skin infections
- •Laboratorytests revealing abnormal Sézary syndrome cells circulating in blood
Lymph node changes include:
- •Enlargedlymph nodes, particularly in neck, armpits, and groin
- •Swellingthat persists or progressively worsens
- •Sometimestenderness in affected nodes
Systemic symptoms many patients experience:
- •Low-grade fever without obvious infection
- •Unexplainedweight loss
- •Nightsweats drenching bedclothes
- •Generalsense of feeling unwell (malaise)
The combination of widespread red skin, severe itching, and enlarged lymph nodes should prompt consideration of Sézary syndrome, particularly in older adults.
Sézary syndrome rash and skin changes
The Sézary syndrome rash is distinctive and often the most distressing symptom patients experience. Erythroderma means red skin covering nearly your entire body. Unlike typical rashes affecting specific areas, this redness is diffuse and persistent. Your skin might look sunburned but without sun exposure. The redness intensifies over time if untreated. What starts as patchy redness progresses to involve larger skin areas, eventually covering 80-90% of your body surface. Scaling accompanies the redness. Your skin constantly sheds scales, covering clothes and bedding. This scaling differs from normal dry skin, being more persistent and extensive. Itching (pruritus) is often the most debilitating symptom. It's not mild discomfort you can ignore. It's intense, relentless itching that keeps you awake at night, interferes with work and relationships, and significantly affects quality of life. Skin thickening (lichenification) develops from chronic scratching and disease progression. Your skin becomes leathery, particularly on hands and feet. Temperature regulation becomes difficult as diseased skin loses normal function. Many patients feel constantly cold or experience inappropriate sweating.
Causes of Sézary syndrome
Understanding Sézary syndrome causes helps address the question every patient asks: "Why did this happen to me?"
Sézary syndrome results from genetic mutation cancer affecting T-cells. These mutations cause cells to multiply uncontrollably and avoid normal cell death. However, doctors are yet to fully understand what causes the mutation.
Environmental triggers haven't been definitively identified. Unlike some cancers with clear environmental causes (smoking and lung cancer, for example), no specific exposures consistently linked to Sézary syndrome have been found. Chronic immune stimulation might contribute. Some researchers theorise that prolonged immune system activation from infections or inflammation may trigger malignant transformation in susceptible individuals, though this remains speculative.
What are the Sézary syndrome risk factors
Sézary syndrome risk factors aren't as clearly defined as risk factors for more common cancers, but certain associations exist. Identified risk factors include:
- •Age over 60:The condition rarely affects younger individuals, with median diagnosis age around 65-70 years
- •Male gender:Men develop Sézary syndrome approximately twice as often as women
- •Previous mycosis fungoides:Some patients with this related T-cell lymphoma progress to Sézary syndrome
- •Chronic immune stimulation:Long-standing inflammatory skin conditions might theoretically increase risk, though evidence is limited
- •Family history:While not clearly hereditary, rare families show clustering of T-cell lymphomas
What's reassuring is that most risk factors aren't modifiable. This isn't a cancer you could have prevented through different lifestyle choices. It's simply an unfortunate occurrence of rare disease.
Sézary syndrome diagnosis
Sézary syndrome diagnosis requires a combination of clinical findings and laboratory confirmation. Multiple tests work together to establish a definitive diagnosis. Diagnostic criteria (Sézary syndrome criteria) include:
- 1. Clinical assessment: Your doctor evaluates skin involvement extent, checking if erythroderma covers sufficient body surface area. They examine lymph nodes and assess systemic symptoms.
- 2. Blood tests reveal: Complete blood count often shows elevated white blood cells. Flow cytometry identifies abnormal T-cells in blood. Sézary syndrome cells have characteristic appearance under microscopy, including cerebriform (brain-like) nuclear contours. T-cell receptor gene rearrangement studies confirm these cells are clonal (all derived from single abnormal cell).
- 3. Skin biopsy provides: Tissue samples from affected skin examined by pathologists. Immunohistochemistry identifies specific markers on abnormal T-cells. This confirms cutaneous T-cell lymphoma diagnosis.
- 4. Lymph node biopsy when indicated:If lymph nodes are significantly enlarged, biopsy determines if lymphoma has spread there. This affects staging and treatment planning.
- 5. Imaging studies include: CT scans evaluating lymph nodes throughout body. PET scans are sometimes used to assess disease extent and metabolic activity.
Diagnosis requires demonstration of erythroderma, circulating atypical T-cells meeting specific thresholds, and confirmation these cells are clonal malignant population.
Sézary syndrome treatment
The treatment aims to control disease, relieve symptoms, and improve quality of life. Because this is rare cancer, treatment often occurs at specialised centres. Treatment approaches typically combine multiple therapies: Skin-directed treatments provide symptom relief:
- •Topicalcorticosteroids reduce inflammation and itching
- •Phototherapy(particularly extracorporeal photopheresis) treats circulating abnormal cells
- •Topicalchemotherapy like mechlorethamine applied directly to skin
- •Totalskin electron beam radiation therapy for extensive skin involvement
Systemic therapies target disease throughout body:
- •Oralmedications like bexarotene (retinoid targeting T-cells)
- •Interferon-alfa injections boosting immune response against cancer
- •Chemotherapycombinations for more aggressive disease
- •Immunotherapyincluding mogamulizumab (antibody targeting specific marker on Sézary cells)
- •Newertargeted therapies like histone deacetylase inhibitors
Supportive care addresses symptoms:
- •Antihistaminesand other medications controlling severe itching
- •Emollientsmaintaining skin moisture and reducing scaling
- •Antibioticstreating skin infections
- •Nauseamedications if chemotherapy is used
- •Painmanagement and fatigue support
Key takeaways
Sézary syndrome is a rare aggressive T-cell lymphoma causing widespread red skin rash, severe itching, and abnormal lymphocytes circulating in blood. While Sézary syndrome cure remains elusive, modern treatments significantly improve quality of life and can achieve disease control for extended periods. Additionally, Sézary syndrome life expectancy varies widely depending on disease characteristics, treatment response, and individual factors. Some patients live many years with good quality of life through ongoing treatment. Living with rare cancer feels isolating, but you're not alone. Support exists through specialist centres, patient advocacy groups, and multidisciplinary teams experienced in managing this complex condition. For comprehensive evaluation and treatment of cutaneous lymphomas including Sézary syndrome, connect with experienced oncology specialists at centres familiar with rare cancers who can provide expert care and access to latest therapies.
FAQs
Related Blogs


Recognising the Signs of Cancer in the body that often go unnoticed