
Uterine Cancer
What is Uterine Cancer?
Uterine cancer originates in the uterus, the pear-shaped organ where fetal development occurs during pregnancy. It is the most common gynecological cancer in women and typically affects postmenopausal individuals. The two primary types are endometrial carcinoma and uterine sarcoma.
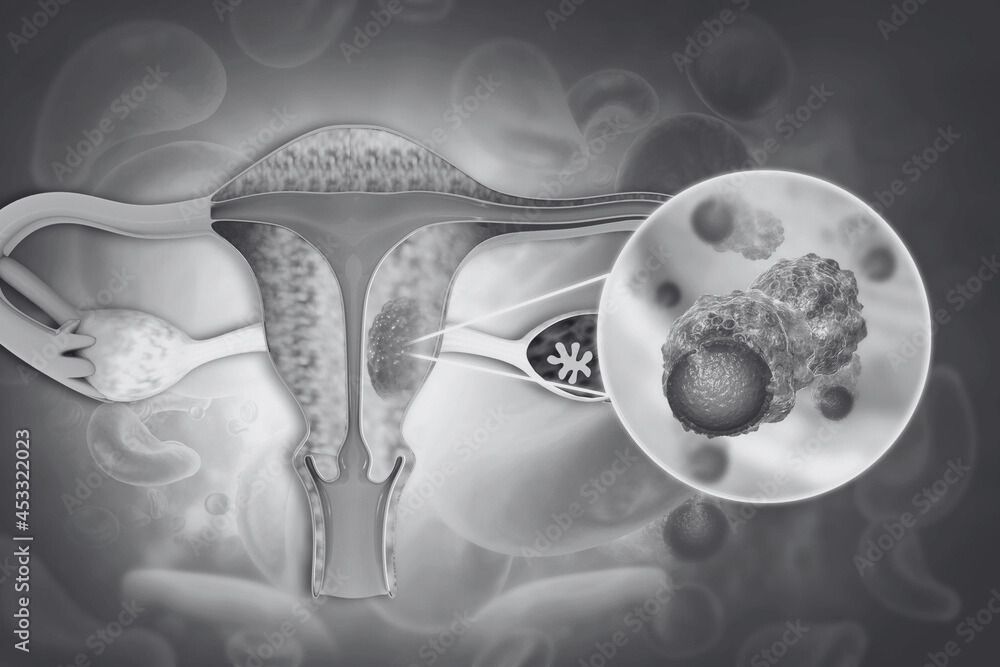
Uterine Cancerr Types
Endometrial Carcinoma
•Most common type, starts in the lining of the uterus (endometrium) and often occurs with a history of unusual vaginal bleeding. Most tumors are caught early and have excellent results with surgery and/or radiation.
Uterine Sarcoma
•A rarer, more aggressive form that grows in the muscle or connective tissue of the uterus. It grows and spreads faster than endometrial cancer, typically requiring vigorous treatments like surgery, chemotherapy, and radiation.
Uterine Cancer Symptoms
- •The most frequent sign bleeding after menopause, between periods, or unusually heavy menstrual flow.
What’s Notable
Early diagnosis has an excellent prognosis in most cases.
Most common and earliest sign of abnormal vaginal bleeding.
Obesity and unopposed estrogen exposure are important risks.
Genetic syndromes like Lynch Syndrome increase risk considerably.
Most of them are hormone-sensitive and can be treated with endocrine therapy.
When to Seek Help
You should consult a gynecologist or oncologist if you experience abnormal vaginal bleeding, especially after menopause or between periods, as it is the most common warning sign of uterine cancer. Seek medical attention if you notice unusual vaginal discharge, persistent pelvic pain or pressure, pain during intercourse or urination, or unexplained weight loss and fatigue. Early evaluation of these symptoms is crucial, as timely diagnosis greatly improves treatment outcomes and long-term recovery.
Uterine Cancer Causes & Risk Factors
Obesity and Diabetes
Increases estrogen exposure and insulin resistance, both of which raise risk.
Early Menstruation/Late Menopause
Increased endometrial growth due to prolonged estrogen exposure.
Hormone Replacement Therapy (unopposed estrogen
Hormone Replacement Therapy (unopposed estrogen
Lynch Syndrome or Genetic Predisposition
Much increased lifetime risk in the presence of inherited mutations.
Age Over 50
Most common affected age group among postmenopausal women.
Never Having Children
Decreased progesterone-dominant cycles may increase risk slightly.
Uterine Cancer Diagnosis
Early Symptoms & Check Up
Step 1: Initial Symptoms & Check-up
Symptoms: Painless neck lump, hoarseness, swallowing difficulty, or persistent neck pain. Physician: clinical neck exam, history review and referral for imaging if suspicious.
Your role: Share any changes you’ve noticed openly.
Uterine Cancer Treatment
Chemotherapy
What it does:
Destroys fast-growing cancer cells all over the body.
Treated for:
Aggressive, recurrent, or violent types like uterine sarcoma.
Recovery:
Side effects are tiredness, queasiness, and hair loss; given in cycles.
Hormonal Therapy
What it does :
Stops estrogen or progesterone to slow down hormone-sensitive cancer growth.
Treated for:
Low-grade, hormone-receptor positive cancers.
Common medications:
Medroxyprogesterone, Tamoxifen, Letrozole.
Recovery:
Milder side effects compared to chemo; frequent checkups necessary.
Targeted Therapy
What it does:
Specialized assault on cancer-specific proteins or genetic mutations.
Treated for:
Advanced cancer with genetic mutations (e.g., HER2+, PI3K pathway).
Drugs used:
Trastuzumab, Everolimus.
Recovery:
Tailored; often paired with hormonal or chemo.
Immunotherapy
What it does:
Boosts the immune system to destroy cancer cells.
Used for:
High MSI or mismatch repair deficient advanced cases.
Drugs used:
Pembrolizumab, Dostarlimab.
Recovery:
Monitored for immune side effects like fatigue or inflammation.
Management & Prevention
Medication Management
•Lifelong thyroid hormone replacement (levothyroxine) to maintain metabolism and prevent recurrence.
Regular Follow-ups
•Routine TSH, T3, T4 tests and neck ultrasounds to monitor hormone levels and detect recurrence early.
Post-Surgical Care
•Wound care, calcium monitoring, and voice rehabilitation if nerve involvement occurred.
Nutrition & Lifestyle
•Balanced diet with sufficient protein, iodine, and antioxidants; stay hydrated and avoid smoking or excessive soy.
Uterine Cancerr Types
Endometrial Carcinoma
•Most common type, starts in the lining of the uterus (endometrium) and often occurs with a history of unusual vaginal bleeding. Most tumors are caught early and have excellent results with surgery and/or radiation.
Uterine Sarcoma
•A rarer, more aggressive form that grows in the muscle or connective tissue of the uterus. It grows and spreads faster than endometrial cancer, typically requiring vigorous treatments like surgery, chemotherapy, and radiation.
Uterine Cancer Symptoms
- •The most frequent sign bleeding after menopause, between periods, or unusually heavy menstrual flow.
What’s Notable
Early diagnosis has an excellent prognosis in most cases.
Most common and earliest sign of abnormal vaginal bleeding.
Obesity and unopposed estrogen exposure are important risks.
Genetic syndromes like Lynch Syndrome increase risk considerably.
Most of them are hormone-sensitive and can be treated with endocrine therapy.
When to Seek Help
You should consult a gynecologist or oncologist if you experience abnormal vaginal bleeding, especially after menopause or between periods, as it is the most common warning sign of uterine cancer. Seek medical attention if you notice unusual vaginal discharge, persistent pelvic pain or pressure, pain during intercourse or urination, or unexplained weight loss and fatigue. Early evaluation of these symptoms is crucial, as timely diagnosis greatly improves treatment outcomes and long-term recovery.
Uterine Cancer Causes & Risk Factors
Obesity and Diabetes
Increases estrogen exposure and insulin resistance, both of which raise risk.
Early Menstruation/Late Menopause
Increased endometrial growth due to prolonged estrogen exposure.
Hormone Replacement Therapy (unopposed estrogen
Hormone Replacement Therapy (unopposed estrogen
Lynch Syndrome or Genetic Predisposition
Much increased lifetime risk in the presence of inherited mutations.
Age Over 50
Most common affected age group among postmenopausal women.
Never Having Children
Decreased progesterone-dominant cycles may increase risk slightly.
Uterine Cancer Diagnosis
Early Symptoms & Check Up
Step 1: Initial Symptoms & Check-up
Symptoms: Painless neck lump, hoarseness, swallowing difficulty, or persistent neck pain. Physician: clinical neck exam, history review and referral for imaging if suspicious.
Your role: Share any changes you’ve noticed openly.
Uterine Cancer Treatment
Chemotherapy
What it does:
Destroys fast-growing cancer cells all over the body.
Treated for:
Aggressive, recurrent, or violent types like uterine sarcoma.
Recovery:
Side effects are tiredness, queasiness, and hair loss; given in cycles.
Hormonal Therapy
What it does :
Stops estrogen or progesterone to slow down hormone-sensitive cancer growth.
Treated for:
Low-grade, hormone-receptor positive cancers.
Common medications:
Medroxyprogesterone, Tamoxifen, Letrozole.
Recovery:
Milder side effects compared to chemo; frequent checkups necessary.
Targeted Therapy
What it does:
Specialized assault on cancer-specific proteins or genetic mutations.
Treated for:
Advanced cancer with genetic mutations (e.g., HER2+, PI3K pathway).
Drugs used:
Trastuzumab, Everolimus.
Recovery:
Tailored; often paired with hormonal or chemo.
Immunotherapy
What it does:
Boosts the immune system to destroy cancer cells.
Used for:
High MSI or mismatch repair deficient advanced cases.
Drugs used:
Pembrolizumab, Dostarlimab.
Recovery:
Monitored for immune side effects like fatigue or inflammation.
Management & Prevention
Medication Management
•Lifelong thyroid hormone replacement (levothyroxine) to maintain metabolism and prevent recurrence.
Regular Follow-ups
•Routine TSH, T3, T4 tests and neck ultrasounds to monitor hormone levels and detect recurrence early.
Post-Surgical Care
•Wound care, calcium monitoring, and voice rehabilitation if nerve involvement occurred.
Nutrition & Lifestyle
•Balanced diet with sufficient protein, iodine, and antioxidants; stay hydrated and avoid smoking or excessive soy.
Why Choose Everhope Uterine Cancer?
At Everhope Oncology, every patient becomes a part of our healing circle—a circle built on trust, expert care, and unwavering support. Uterine cancer care can be complex, but you’re never walking alone.
4th
most common cancer in women worldwide.
90%
endometrial carcinoma.
80%
5+ year survival rate
Explore Our Latest Updates

एमआरआई क्या होता है (MRI Kya Hota Hai): कब और क्यों किया जाता है

Real Breast Cancer Survivor Stories of Courage, Hope and Recovery
FAQs on Uterine Cancer
No question is too small when it comes to your care
Find a Centre Near You
Gurgaon EBD 65
EBD 65, Sector 65, Golf Course Extension Road, Gurgaon
