Pancreatic Neuroendocrine Tumor: Causes, Symptoms & Treatment
Does your blood sugar keep dropping without warning? Sweating, shaking, confusion - then it passes. After the third emergency room visit in two months, imaging reveals a pancreatic mass. Surprisingly, it's not the aggressive pancreatic cancer everyone fears.
Let's explore what makes these tumours unique.
What is a pancreatic neuroendocrine tumour?
Pancreatic neuroendocrine tumour definition centres on their origin: specialised hormone-producing cells scattered throughout the pancreas. When these turn malignant, they create tumours that behave nothing like conventional adenocarcinoma.
The critical distinction lies in growth patterns. Whilst typical pancreatic malignancies spread aggressively within months, neuroendocrine variants often progress slowly over years.
These account for approximately 1-2% of all pancreatic malignancies. Pancreatic neuroendocrine tumour location matters significantly as they develop anywhere within the pancreas (head, body, or tail). However, the location influences symptoms and surgical accessibility.
Types of pancreatic neuroendocrine tumours
Tumour variants are split into two major categories based on hormone production. This distinction profoundly impacts presentation and diagnosis.
Functional tumours create obvious symptoms
These actively secrete hormones, creating dramatic symptoms prompting earlier diagnosis. Insulinomas cause dangerous hypoglycaemia, where patients wake at night drenched in sweat, confused, and sometimes experiencing seizures from low blood sugar.
Functional tumours include:
- •InsulinomasLow blood sugar episodes during fasting or exercise, often requiring frequent carbohydrate consumption
- •GastrinomasSevere heartburn, diarrhoea, stomach ulcers (Zollinger-Ellison syndrome)
- •GlucagonomasCharacteristic rash (migratory necrolytic erythema), weight loss, diabetes
- •VIPomasProfuse watery diarrhoea causing severe dehydration, dangerously low potassium
These obvious symptoms paradoxically benefit patients as the body signals problems whilst tumours remain small and potentially curable. The dramatic hormone-driven presentation typically prompts evaluation within months.
Non-functional tumours hide longer
Comprising 60-90% of cases, these produce no active hormones. They grow silently until size causes mechanical problems - pressing on bile ducts, invading structures, or spreading to lymph nodes and liver.
By discovery, non-functional tumours often measure several centimetres and may have metastasised, worsening prognosis compared to functional counterparts caught early.
Verrucous pancreatic neuroendocrine tumour
What is verrucous pancreatic neuroendocrine tumour? Honestly, this likely represents confusion between different cancer terminologies.
Verrucous describes a warty, cauliflower-like appearance typically seen in skin or mucosal cancers (such as oral or genital sites), not pancreatic tumours.
Pancreatic neuroendocrine tumours don't develop verrucous growth patterns, but they form solid masses within pancreatic tissue.
Recognising pancreatic neuroendocrine tumour symptoms
Pancreatic neuroendocrine tumour symptoms vary dramatically between functional and non-functional types.

Functional tumour symptoms appear early
Hormone-driven symptoms create obvious patterns:
- •Hypoglycaemia episodesWeakness, sweating, confusion, hunger between meals or during sleep
- •Severe heartburn and ulcersPersistent despite acid-reducing medications
- •Watery diarrhoeaProfuse, unrelenting, causing dangerous dehydration
- •Distinctive skin rashMigratory necrolytic erythema in glucagonoma patients
- •Flushing and nauseaParticularly with certain hormone-secreting variants
Non-functional tumour symptoms emerge late
Without hormone clues, symptoms remain non-specific until tumours grow large:
- •Abdominal painPersistent discomfort in the upper abdomen or back
- •JaundiceYellowing skin when head tumours block the bile ducts
- •Weight lossUnexplained, progressive
- •Cancer fatigueProfound exhaustion unrelieved by rest
- •Digestive changesNew-onset diabetes, altered bowel habits
These signs of cancer apply to numerous conditions, explaining diagnostic delays.
Early versus advanced presentations
Early-stage disease often produces no symptoms and is discovered incidentally during imaging.
Advanced disease announces itself through metastatic pancreatic neuroendocrine tumour complications, such as liver masses, extensive abdominal spread, or distant metastases
Understanding pancreatic neuroendocrine tumour causes
Pancreatic neuroendocrine tumour causes remain frustratingly unclear for most cases. Unlike smoking's clear link to lung cancer, these develop without obvious environmental triggers.
Genetic factors dominate known risks
Several inherited syndromes dramatically increase risk:
- •Multiple Endocrine Neoplasia type 1 (MEN1)This genetic syndrome causes tumours in multiple hormone glands. Pancreatic neuroendocrine tumours develop in 30-80% of MEN1 patients . Families carrying MEN1 mutations require lifelong screening.
- •Von Hippel-Lindau disease, Neurofibromatosis type 1, Tuberous sclerosisThese hereditary conditions also elevate risk.
These genetic syndromes explain perhaps 10-15% of cases. The remaining 85-90% arise sporadically without identifiable cause.
Sporadic versus inherited patterns
Primary pancreatic neuroendocrine tumour development without family history remains unpredictable. No lifestyle modifications have been demonstrably shown to reduce risk because we don't understand what initiates transformation.
This uncertainty frustrates patients seeking explanations. Unlike cancer risk factors for common malignancies, these appear randomly, emphasising the importance of early detection when symptoms emerge.
How doctors diagnose pancreatic neuroendocrine tumours
Pancreatic neuroendocrine tumour diagnosis requires systematic investigation combining clinical assessment, biochemical testing, and advanced imaging.
Tests used to confirm diagnosis
Blood tests establish biochemical diagnosis for functional tumours:
- •Hormone levels(insulin, gastrin, glucagon, VIP)
- •Chromogranin A(general marker)
- •Standard blood counts
Imaging modalities visualise tumours:
- •CT scansProvide detailed pancreatic anatomy, detecting masses and evaluating spread to liver or regional nodes.
- •MRIOffers superior soft tissue contrast, particularly for detecting small liver metastases missed on CT.
- •PET scansSpecifically targets somatostatin receptors abundant in neuroendocrine tumours. This functional imaging detects disease that conventional scans miss, particularly critical for advanced disease staging.
- •Endoscopic ultrasoundProvides high-resolution pancreatic imaging, allowing simultaneous biopsy.
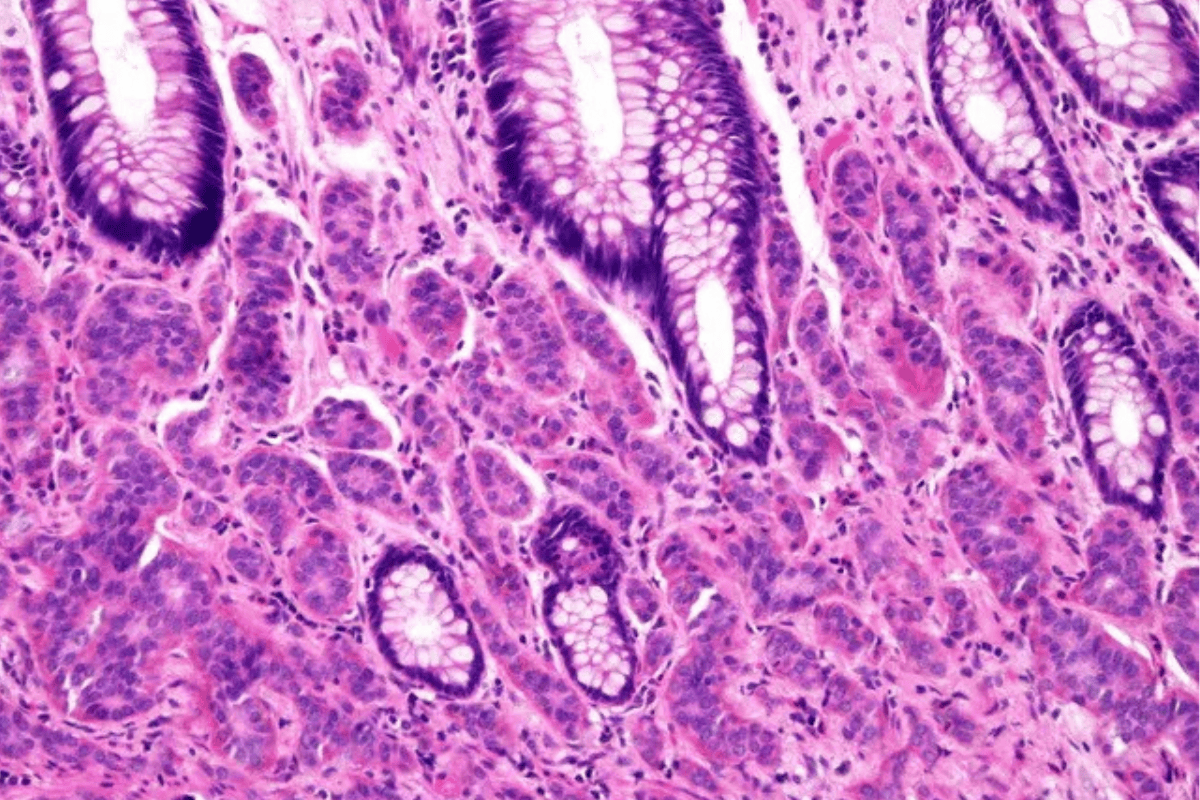
A biopsy confirms the diagnosis definitively through fine-needle aspiration, which obtains cells for microscopic examination and grade determination.
Understanding pancreatic neuroendocrine tumour grading and staging
Pancreatic neuroendocrine tumour grading assesses tumour aggressiveness while staging maps disease extent.
Tumour grades predict behaviour
Grading examines cellular proliferation through mitotic count and Ki-67 index.
- •Grade 1 (Low grade)Mitotic count under 2 per 10 fields, Ki-67 under 3%. Slow growth, favourable prognosis.
- •Grade 2 (Intermediate grade)Mitotic count 2-20, Ki-67 3-20%. Moderate growth, intermediate metastatic potential.
- •Grade 3 (High grade)Mitotic count over 20, Ki-67 over 20%. Aggressive behaviour, rapid growth, early spread, poor outcomes.
Stages of pancreatic neuroendocrine tumour
Stages of cancer classification follows TNM system:
- •LocalisedTumour confined to pancreas, no lymph node involvement, no distant spread. Surgery offers a potential cure.
- •RegionalTumour extends into nearby structures or involves regional nodes. Surgery remains possible, but outcomes depend on the extent and feasibility of complete removal.
- •MetastaticDisease spreads to the liver, lung, bone, or distant sites. Cure becomes unlikely, treatment focuses on control and symptom management. However, even Stage IV disease allows years of survival with appropriate therapy.
Treatment approaches for pancreatic neuroendocrine tumours
Pancreatic neuroendocrine tumour treatment varies dramatically based on functional status, grade, stage, and patient factors.
Surgery remains the primary option for localised disease. Complete surgical removal offers only a curative option:
- •EnucleationShelling out small, superficial tumours
- •Partial pancreatectomyRemoving the portion containing the tumour
- •Whipple procedureComplex operation for head tumours
Surgery carries risks, such as pancreatic leak, diabetes, and digestive enzyme insufficiency. However, complete removal of low-grade tumours frequently achieves long-term survival.
When surgery isn't feasible, go for these medical therapies:
- •Somatostatin analoguesOctreotide and lanreotide control hormone secretion and slow tumour growth.
- •Targeted therapiesEverolimus and sunitinib demonstrated survival benefits in advanced disease.
- •Peptide receptor radionuclide therapy (PRRT)Lutetium-177 dotatate delivers targeted radiation, significantly improving progression-free survival.
- •ChemotherapyReserved for higher-grade tumours progressing despite other treatments.
- •Liver-directed therapiesFor liver-dominant metastases, providing local control.
Pancreatic Neuroendocrine Tumour Survival Rate & Life Expectancy
Pancreatic neuroendocrine tumour cure remains possible for early-stage, low-grade tumours completely removed surgically. However, most face chronic disease management rather than a cure.
Even an incurable disease often allows years of good-quality life. Pancreatic neuroendocrine tumours survival rate varies enormously:
- •Localised low-grade90-95% five-year survival
- •Localised high-grade50-60% five-year survival
- •Metastatic low-grade60-70% five-year survival
- •Metastatic high-grade15-20% five-year survival
These dramatically exceed conventional adenocarcinoma survival, highlighting why accurate diagnosis matters so much.
Getting the Best Guidance for Pancreatic Neuroendocrine Tumour
Receiving this diagnosis triggers understandable anxiety, but understanding the disease's nature helps frame realistic expectations.
- •FirstConfirm you're receiving care from specialists experienced with neuroendocrine tumours. Seek centres with dedicated programmes where multidisciplinary teams collaborate regularly.
- •SecondEnsure complete staging occurred. Gallium-68 dotatate PET-CT should be standard, detecting disease that conventional imaging misses.
- •ThirdIf a functional tumour causes symptoms, pursue symptom control aggressively. Somatostatin analogues can dramatically improve quality of life.
- •FinallyMaintain hope tempered with realism. Even advanced disease allows years of productive life with appropriate cancer treatment . Focus on quality, managing symptoms, maintaining function, rather than fixating exclusively on cure.
FAQs
Related Blogs