
Prostate Infection Explained: Symptoms, Causes & Treatment
Frequent bathroom trips at night, a dull ache that won't go away, or discomfort that makes even simple tasks feel challenging.
The prostate is a small gland located just beneath the bladder. When it becomes inflamed or infected, it can disrupt your whole life. But it's not a condition without any remedy that can make you feel more comfortable and better.
In this guide,
What is prostatitis meaning?
How to define prostatitis? It is the inflammation of the prostate, a walnut-sized gland that sits just below the bladder in men. It wraps around the urethra, the tube that carries urine out of the body.
Despite its small size, the prostate gland performs several important functions in your body that keep the reproductive system working well.
- •Produces seminal fluidThe prostate creates a milky fluid that mixes with sperm and makes up a large part of semen.
- •Nourishes and protects spermEnzymes, proteins, and minerals in prostatic fluid keep sperm healthy and protect them from bacteria and acidic conditions.
- •Aids ejaculationMuscle fibres in the prostate contract during ejaculation, pushing semen through the urethra and out of the body.
- •Supports urinary functionIt surrounds the urethra just below the bladder, so changes in its size or structure can affect urine flow.
4 types of prostatitis: What you need to know about them?
There are actually different prostate infection reasons, and each one has its own characteristics. A prostatitis specialist evaluates which type you have to determine the most effective treatment approach.

Let's explore each type in detail so you can recognise the differences and understand them better.
1. Acute bacterial prostatitis
This is the least common but most severe type of prostate infection. It occurs when bacteria suddenly invade the prostate tissue, causing a rapid infection. The condition develops quickly and needs immediate medical attention with medication to prevent serious complications.
2. Chronic bacterial prostatitis
Chronic bacterial prostatitis happens when a bacterial infection in the prostate won't go away or keeps returning. The bacteria settle deep in the prostate tissue, making them hard to eliminate completely.
You will need to take antibiotics for an extended period, often several weeks to months, to resolve the infection fully.
3. Chronic prostatitis/chronic pelvic pain syndrome (CPPS)
This is the most common type of prostatitis and also the most complex to diagnose. No bacterial infection is present, yet inflammation occurs in the prostate or the surrounding pelvic area.
It can be because of nerve issues, muscle tension, immune system responses, or previous injuries to the pelvic region.
4. Asymptomatic inflammatory prostatitis
In this condition, inflammation is in the prostate but does not cause any noticeable signs. It's usually discovered accidentally during a prostatitis test or routine screening for other health concerns.
The inflammation shows up in lab results or tissue samples, but it doesn't affect your daily life or require treatment in most cases.
What is the most common cause of prostatitis? Signs to watch for
The symptoms you experience depend on the specific type and the severity of the inflammation or infection.

Recognising these signs of prostatitis early can help you receive the care you need promptly.
1. Pain or burning during urination
One of the most common symptoms is discomfort while urinating. You might feel a sharp burning sensation or stinging pain as urine passes through the urethra. This happens because the inflamed prostate puts pressure on the urethra and irritates surrounding tissues.
2. Pelvic and lower back pain
Prostatitis pain often shows up in the pelvic region or lower back, ranging from a dull ache to sharp, persistent pain. When inflammation in the prostate affects nearby muscles, nerves, and tissues, it leads to this widespread discomfort.
3. Pain in the groin or genital area
You might experience pain in your groin, testicles, or the area between your scrotum and rectum. This pain can be constant or come and go throughout the day. It’s because the prostate sits close to these areas that inflammation spreads outward and causes discomfort in multiple spots.
4. Fever and fatigue in severe infections
When prostate inflammation is caused by bacteria, you may experience fever, nausea and chills. Your body fights the infection, which leaves you feeling exhausted and weak. These symptoms need prompt medical attention and prostatitis medication.
Prostate infection causes: Key risk factors to know
Once you know what causes prostatitis, you can spot the warning signs and get proper care. The reasons for infection vary depending on the type, but several factors can trigger inflammation or infection in the prostate gland.
Bacterial infection in the prostate gland
Bacteria from the urinary tract can travel backward and enter the prostate tissue. Once inside, these bacteria multiply and cause infection, leading to acute or chronic bacterial prostatitis. E. coli is the most common cause of prostatitis in bacterial cases.
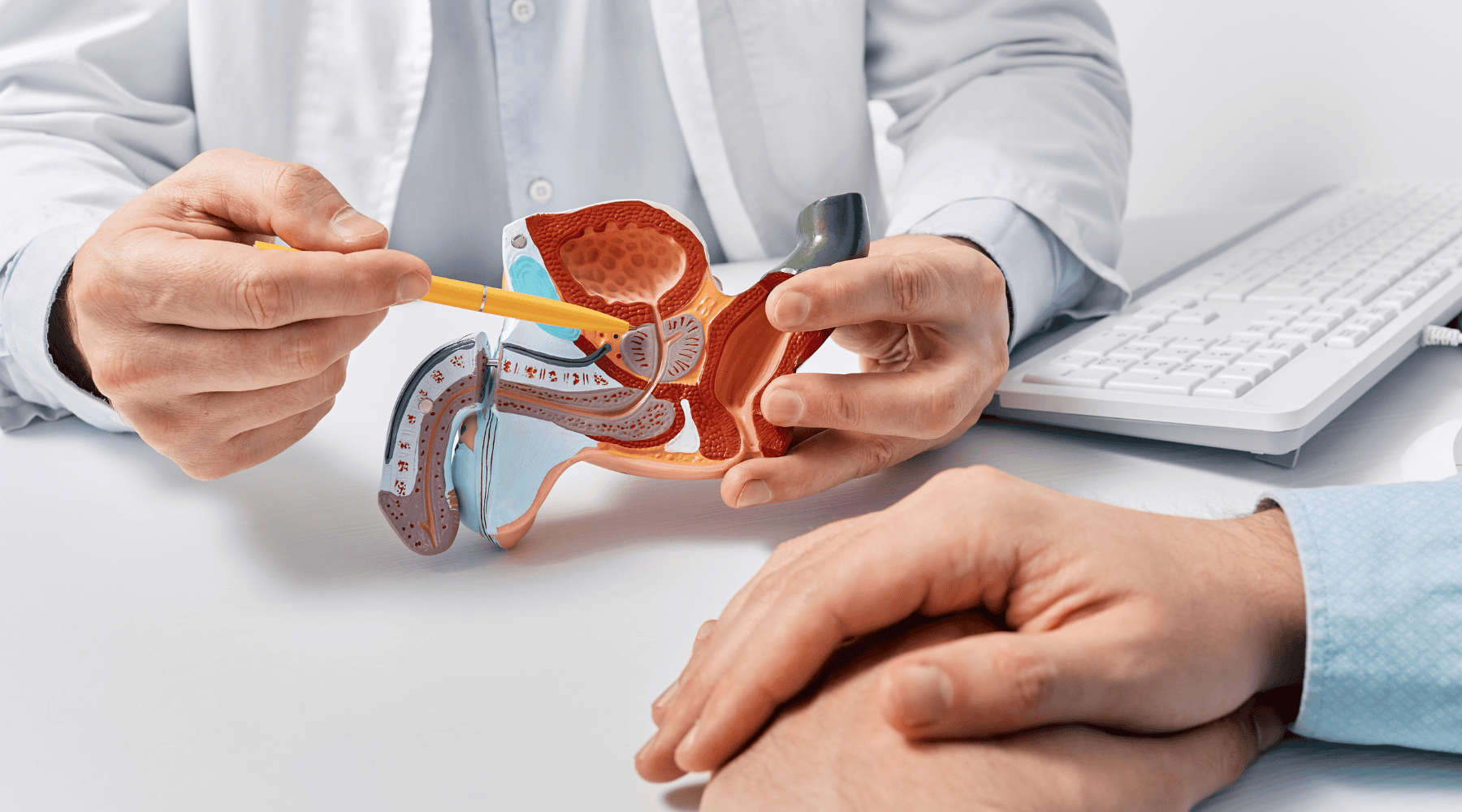
Urinary tract infections leading to inflammation
A urinary tract infection or bladder infection can spread to the prostate gland if left untreated. The bacteria move from the bladder or urethra into the prostate, triggering inflammation and symptoms of prostate infection.
With that being said, men with recurring UTIs face a higher risk of developing prostatitis.
Nerve or muscle damage in the pelvic region
Injury or strain to the pelvic floor muscles can contribute to chronic prostatitis. Nerve damage from previous surgeries, trauma, or chronic tension affects how the prostate functions. This type of damage often leads to chronic pelvic pain syndrome rather than bacterial infection.
How to treat prostatitis: Effective remedies that help with discomfort
Let’s take a look at these treatments that can help:
- •Antibiotics for bacterial infections:If bacteria cause your prostatitis, antibiotics are the primary medicine for prostatitis infection. Acute infections typically need two to four weeks of medication, while chronic cases may require several weeks to months of treatment.
- •Pain relievers and anti-inflammatory drugs:Over-the-counter medications can help reduce inflammation and ease the pain of prostatitis. Your doctor may prescribe stronger pain medication if symptoms are severe.
- •Alpha-blockers:These medications relax the muscles around the prostate and the bladder neck. They help improve urine flow and reduce discomfort during urination, which is common in prostatitis symptoms.
- •Physical therapy:Pelvic floor physical therapy can help alleviate pain if muscle tension is contributing to your discomfort. A therapist teaches you exercises to relax tight muscles and improve pelvic floor function.
- •Warm sitz baths:Soaking in warm water for 15-20 minutes can provide relief from pelvic pain. The warmth relaxes muscles and reduces inflammation in the prostate area.
- •Lifestyle changes:Avoiding caffeine, alcohol, and spicy foods may help reduce bladder irritation. Staying hydrated and exercising regularly also supports overall prostate health and recovery.
Diagnosing prostate infection: What to expect

Additionally, urine tests can detect bacteria or white blood cells that point toward infection. Blood tests may also be ordered to check for signs of infection or inflammation in your body.
Your doctor might recommend a prostate infection test that analyses prostatic fluid or semen samples for a clearer diagnosis.
Final words: Prevention and long-term care
Prostatitis can be challenging, but that doesn't mean you have to live your life with discomfort. Some medications and remedies can help manage an acute prostate gland infection effectively.
Staying well hydrated helps flush out bacteria and supports your urinary system. Following your doctor's advice and completing your course of antibiotics prevents the infection from returning. Additionally, warm sitz baths can offer relief from pelvic pain and reduce inflammation.
With a chronic condition,
Pay attention to how your body feels and don't hesitate to reach out for support when symptoms change. Remember, you're not alone in this, and taking the right steps can make a real difference.
FAQs on prostatitis
Related Blogs

What Is Enlarged Prostate (BPH)? Signs, Diagnosis and Treatment


