Urothelial Carcinoma Explained: Symptoms, Causes, and Treatment
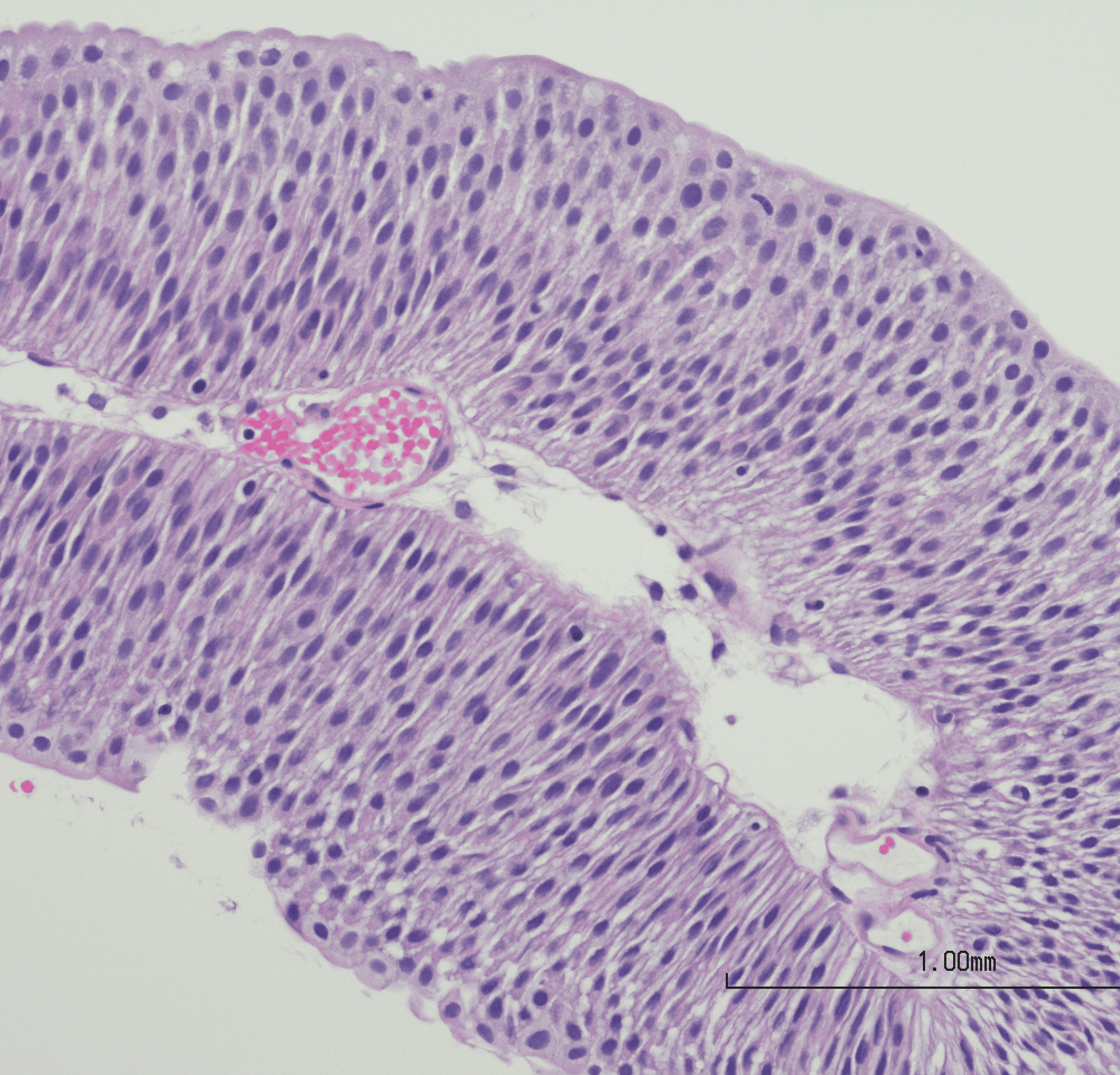
Sometimes, it begins with a small change that does not seem urgent. A symptom may come and go, easy to ignore at first.
Then a term like urothelial carcinoma appears, and with it, uncertainty. Feeling unsettled at this stage is natural. Taking time to understand what it means can help ease some of that burden.
Urothelial carcinoma is a cancer that affects the lining of the urinary system, most often the bladder. It can develop gradually, and with timely care, many cases can be managed effectively.
In this blog, we’ll explain what urothelial carcinoma means, its symptoms, causes, and treatment options, so you and your family can move forward with clarity and care.
What is urothelial carcinoma?
If you have been wondering about urothelial carcinoma meaning, it refers to abnormal cell growth in this specialised lining that normally helps store and transport urine. It is one of the types of cancer that begins in the urothelial cells lining the urinary system.

It most commonly affects:
- •The bladder (bladder urothelial carcinoma)
- •The ureters (tubes connecting the kidneys to the bladder)
- •The renal pelvis (part of the kidney where urine collects)
In most cases, it develops when DNA mutations cause these cells to grow and divide in an uncontrolled manner. Over time, this can lead to tumour formation within the lining.
Urothelial carcinoma is the most common type of bladder cancer, though it can also occur in other parts of the urinary tract.
2 key urothelial carcinoma types
Types are defined by how deeply the tumour grows and how abnormal the cancer cells appear.
This system, known as the urothelial carcinoma classification, helps guide treatment and understand how the disease may behave.
In simple terms, classification is based on:
- Invasion, which refers to how far the tumour has grown
- Grade, which describes how abnormal the cancer cells look
1. Non-invasive urothelial carcinoma
Non-invasive tumours remain limited to the inner lining and do not grow into deeper layers.
These include:
- •Ta
- •T1
- •Carcinoma in situ (CIS)
They are often associated with low-grade urothelial carcinoma, where cells appear less aggressive and tend to grow slowly. The immediate risk of spread is lower, though ongoing monitoring is still important.
2. Invasive urothelial carcinoma
Invasive tumours grow deeper into the bladder wall and may reach nearby tissues. They are more likely to progress and spread.
High-grade urothelial carcinoma is common in this group, with cells appearing more abnormal and behaving more aggressively.
Important note: Grade describes how the cells behave, while stage reflects how far the cancer has spread in the body.
Urothelial carcinoma symptoms
One of the most common signs is painless blood in urine, which may appear pink, red, or tea-coloured. It can come and go, which is why it is sometimes overlooked.
Other symptoms may include:
- •Frequent urination
- •A strong or sudden urge to urinate
- •Discomfort or pain during urination
- •Pelvic pain in more advanced stages
These changes can feel concerning, but they do not always point to cancer. Many of these signs can also be linked to infections or other urinary conditions, unlike symptoms such as blood in stool, which are usually related to a different part of the body.
In the early stages, the symptoms can be subtle and easy to miss. Noticing persistent changes and discussing them with an oncologist can help ensure the right steps are taken, even if the cause turns out to be something less serious.
Urothelial carcinoma causes
Urothelial carcinoma causes are linked to changes in the DNA of urothelial cells that line the urinary tract. These mutations affect how cells grow and divide, leading to abnormal growth over time.
Changes at the cellular level
- •Mutations develop in urothelial cells
- •These changes disrupt normal cell control
- •Cells begin to grow and multiply abnormally
Role of carcinogens in urine
- •Harmful substances pass through the urinary system
- •Repeated exposure can damage the lining
- •This may trigger a genetic mutation cancer process within the cells
While considering these, it's also important that there is no single cause. Most cases develop over time, and multiple factors may act together. In many situations, there is no clear or direct cause.
Urothelial carcinoma risk factors
Risk factors are linked to long-term exposure to certain conditions and substances that affect the urinary tract.

These factors can increase the likelihood over time. Common risk factors include:
- •Smoking, which is the strongest and most well-established link
- •Occupational exposure to chemicals used in industries such as dyes, rubber, and textiles
- •Increasing age, with a higher risk seen in older adults
- •Male sex, as the condition is more common in men
- •Chronic inflammation of the bladder, often due to infections or irritation
- •Prior treatments such as chemotherapy or radiation involving the pelvic area
These are part of a broader set of cancer risk factors that influence how cells respond to long-term damage. Even when one or more risk factors are present, many people do not develop cancer, and regular monitoring can help detect changes early.
Urothelial carcinoma staging
Staging describes how far the cancer has grown and spread within the body. In simple terms, staging reflects the extent of spread and helps guide treatment decisions.
Doctors often use the TNM system:
- •T refers to how deeply the tumour has grown into the bladder wall
- •N indicates whether nearby lymph nodes are involved
- •M shows whether the cancer has spread to other parts of the body
The staging is usually grouped into stages 0 to IV:
- •Stage 0: Cancer is limited to the inner lining
- •Stage I: Cancer has grown into the connective tissue layer
- •Stage II: Cancer has reached the muscle layer
- •Stage III: Cancer has spread to nearby tissues or organs
- •Stage IV: Cancer has spread to distant parts of the body
Stages III and IV are often referred to as advanced urothelial carcinoma. When the disease spreads to distant organs, it is known as metastatic urothelial carcinoma. This system aligns with broader stages of cancer used across many cancer types.
Diagnosis and tests for urothelial carcinoma
Diagnosis follows a structured process, with each step helping confirm the condition and understand how far it has developed.
The evaluation often begins with:
- •Urine cytology, which looks for abnormal or cancerous cells in a urine sample
- •Additional urine tests to detect markers linked to tumour activity
The next step is:
- •Cystoscopy is the core diagnostic test where an oncologist uses a thin, flexible camera to examine the bladder lining directly
- •This allows any suspicious areas to be identified in real time
To confirm the diagnosis:
- •A biopsy is performed during cystoscopy
- •The tissue sample is examined to determine the presence and type of cancer
Imaging helps assess spread and staging:
- •CT or MRI scans provide detailed views of the urinary tract and nearby structures
- •In selected cases, a PET scan cancer assessment may be used to detect disease beyond the primary site
Together, these tests confirm both the type and stage, guiding the next steps in care.’
3 types of urothelial carcinoma treatment
Treatment for urothelial carcinoma depends on the stage of the cancer and its grade, which reflects how aggressive the cells appear. Treatment is planned carefully to manage the condition while supporting overall well-being.
1. Non-invasive disease
For early-stage tumours, treatment focuses on removing growths and preventing recurrence.
- •TURBT (transurethral resection of bladder tumour) removes visible tumours from the bladder lining
- •Intravesical therapy delivers medication directly into the bladder, often using BCG or chemotherapy
2. Invasive disease
When the cancer grows deeper, treatment becomes more extensive.
- •Cystectomy may involve removing part or all of the bladde
- •Systemic chemotherapy is often used alongside surgery to reduce the risk of spread
3. Advanced disease
In advanced stages, treatment aims to control the disease throughout the body.
- •Immunotherapy helps the immune system recognise and target cancer cells
- •Targeted therapy focuses on specific changes within cancer cells to slow their growth
Treatment for urothelial carcinoma often combines these approaches as part of broader cancer treatment strategies tailored to each situation.
Moving forward with clarity and care
Early detection plays an important role in managing this condition. Symptoms such as blood in urine, even when painless, should be evaluated without delay, as urothelial carcinoma prognosis often improves with timely care.
It is natural to feel overwhelmed while noticing new symptoms. On the bright side, urothelial carcinoma survival rates are generally better when diagnosed early, and support is available at every step.
If you need help understanding your diagnosis or planning next steps, speaking with a specialist can provide clarity. Oncology doctors at Everhope can guide you through your options and support your care journey.
FAQs
Related Blogs


Recognising the Signs of Cancer in the body that often go unnoticed