What Is Extravasation? Understanding This Chemotherapy Complication
An IV line may have become a regular part of your life if you are undergoing cancer treatment. Most of the time, it safely delivers medications, fluids, and chemotherapy drugs into your body to fight the disease.
But sometimes a situation called extravasation can happen.
If you’re hearing this word for the first time, it may sound alarming. For patients receiving cancer therapies, it raises questions: Is extravasation dangerous? How would I know if it happens?
Extravasation is a known complication of IV therapy. While it doesn’t happen often, healthcare teams take it seriously because some medications, especially chemotherapy drugs, can irritate or damage tissue.
With early recognition, proper extravasation management, and effective prevention, most cases can be managed safely.
What is extravasation?
Extravasation is the accidental leakage of IV medication from a vein into the surrounding tissue under the skin.
In IV therapy, a catheter is placed inside a vein so medication flows directly into the bloodstream and travels through the body.
If the catheter shifts or the vein becomes damaged, medication can escape from the vessel wall and spread into nearby tissue.
However, extravasation meaning usually refers to leakage involving chemotherapy drugs that can irritate or damage tissue.
During chemotherapy extravasation, certain drugs can trigger severe inflammation, blistering, and tissue injury if they remain trapped under the skin.
That is why nurses and oncologists monitor infusion sites closely and encourage patients to report unusual sensations immediately.
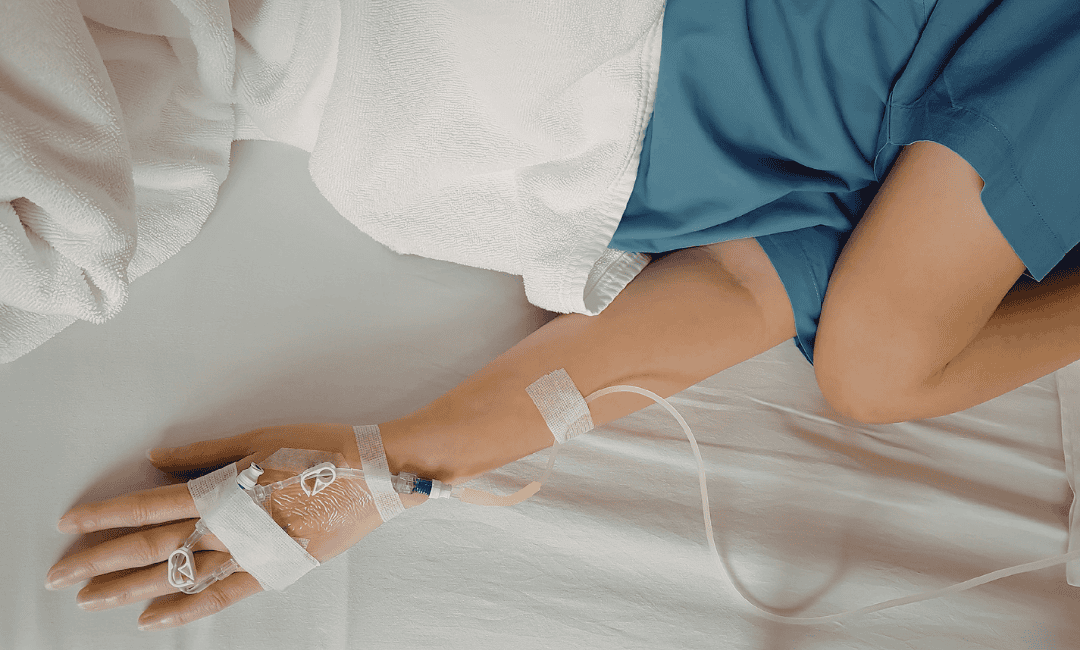
Types of extravasation and how different drugs affect tissue
Not all cases of extravasation are equally dangerous. Some chemotherapy regimens, such as folfox chemotherapy, involve drugs that must be administered carefully through IV therapy.
Pathologists usually classify extravasation based on how harmful the leaked medication is to tissue.
DNA-binding vesicant drugs
Many chemotherapy drugs are vesicants, which means they can damage tissue if leakage occurs. This is why extravasation cancer treatments require careful monitoring.
Some vesicant drugs bind directly to cellular DNA. When they leak into tissue, they can continue damaging cells even after the initial exposure. As damaged cells break down, the drug may be released again into nearby tissue, causing ongoing injury.
These medications can lead to:
- •Blistering
- •Severe inflammation
- •Tissue necrosis
This is why serious extravasation complications can worsen over time if not treated quickly.
Non–DNA–binding vesicants
Non–DNA-binding vesicants are generally less destructive but may still cause:
- •Inflammation
- •Pain
- •Localised tissue injury
Drugs such as vinca alkaloids (vincristine, vinblastine, vinorelbine) block cell division rather than binding to DNA. Because they do not attach to DNA, the body can gradually clear them through the lymphatic system, so the injury usually remains more localised.

Non-vesicant solutions
Some medications are also considered non-vesicants, meaning they usually do not damage tissue if leakage occurs.
For instance, advanced treatments like HIPEC chemotherapy are used in certain cancers and require specialised delivery methods.
When leakage occurs, patients may notice swelling or discomfort, but the body typically absorbs the fluid without serious injury.
Oncologists may describe these cases as mild extravasation, where treatment mainly involves monitoring and supportive care.
Symptoms and common causes of extravasation
The most critical step of extravasation is early recognition, as the window to limit tissue damage is often very small, usually just the first few hours. If oncologists can detect the problem quickly, extravasation treatment can begin before the drug causes deeper injury.
To identify whether extravasation is happening, we usually depend on signs from what the patient feels, what oncologists observe, and how the IV system behaves.
What are extravasation symptoms?
The earliest extravasation symptoms often appear during the infusion. Even you’ve probably noticed the first warning signs, as it happens in most cases.
At this stage, patients and clinicians may notice symptoms such as:
- •Burning or stinging at the injection site
- •Swelling around the IV area
- •Redness or skin discolouration
- •Aching pain along the vein
- •Tightness or pressure under the skin
Another warning sign is the inability to draw blood back through the catheter. When blood cannot return, it may indicate that the catheter is no longer properly positioned in the vein.
If early signs are missed, symptoms may appear later. Over the next hours or days, the area can become more inflamed or firm as the tissue reacts to the leaked medication.
In more severe cases, tissue injury can contribute to cancer pain or discomfort around the infusion site.

What are the causes of extravasation?
Understanding the causes of extravasation helps healthcare teams prevent leakage during IV therapy.
In most cases, this happens because something disrupts the normal function or position of the IV line. When that happens, the medication may no longer flow through the vein and instead enter the surrounding tissue.
Several factors can contribute to this, including:
- Improper IV placement: If the catheter is not fully positioned inside the vein, medication may leak into nearby tissue during the infusion.
- Fragile or damaged veins: If you are older or have undergone repeated IV treatments, you may have weaker veins that are more prone to leakage.
- High-pressure infusions: Rapid delivery of medication can stress your vessel wall and increase the chance of rupture.
- Drug-related irritation: Chemotherapy side effects include irritation and the lining of blood vessels weakening over time.
In many situations, extravasation happens because more than one of these factors occurs at the same time.
Understanding these risks is an important step in preventing extravasation, helping healthcare teams minimise the risk of leakage during IV therapy.
Risk factors that increase the chance of extravasation
The risk of extravasation can increase because of factors related to the patient, the IV procedure, or the medication being given.
Recognising these risks helps healthcare teams plan safer treatment and strengthen extravasation prevention:
| Risk factor | Why it matters |
|---|---|
| Fragile veins | Veins weakened by age, disease, or previous treatments can leak more easily. |
| Difficulty reporting symptoms | Children, elderly patients, or those with nerve damage may not notice or report pain early. |
| Certain health conditions | Conditions such as diabetes or obesity can affect blood vessels and make IV placement harder. |
| IV placed near joints | Areas like the wrist or elbow move frequently, which can shift the catheter. |
| Type of IV line used | Peripheral IV lines generally have a higher chance of leakage than central lines. |
| Long infusion time | Longer infusions increase the chance that the catheter may move or the vein may become irritated. |
| Strong or concentrated drugs | Chemotherapy can cause more severe tissue injury if leakage occurs. |
Diagnosis and tests for extravasation
If your oncologist suspects extravasation, they would often follow established extravasation guidelines when assessing and treating these injuries. While most cases are diagnosed through observation, additional tests might be required as well.
Clinical assessment
The first step in extravasation diagnosis is a physical examination of the IV site. Oncologists and nurses look for swelling, redness, tenderness, or skin colour changes. You might be asked about sensations like burning, pain, or tightness.
Grading the severity
Once extravasation is confirmed, healthcare teams assess how serious the injury is. Most hospitals use the Common Terminology Criteria for Adverse Events (CTCAE) developed by the National Cancer Institute.
To monitor changes, clinicians often mark the edges of redness or swelling on the skin. This helps them see whether the affected area is spreading.
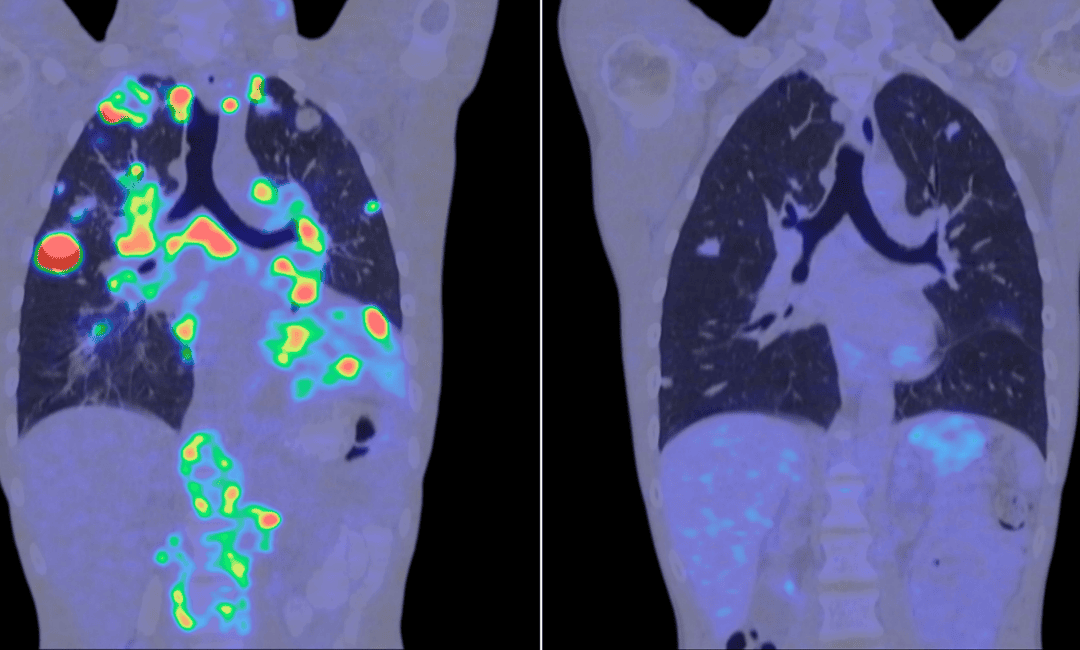
Imaging tests
Imaging tests used to confirm tissue injury are part of broader cancer diagnostics used in oncology care. These tests help determine whether muscles, tendons, or other structures have been affected.
For that, ultrasound can show fluid collections under the skin, while MRI or CT scans provide detailed images of deeper tissue damage when needed.
In complex situations, specialists in interventional oncology may assist with imaging or treatment planning.
Treatment options for extravasation
Immediate extravasation treatment approaches include:
| Step or treatment | What it does |
|---|---|
| Stop the infusion | Stop the IV immediately to prevent further leakage. |
| Leave the catheter in place | Keep the IV line temporarily to remove leaked medication. |
| Aspirate the drug | Use a syringe to withdraw the remaining medication. |
| Remove the catheter | Remove the needle after aspiration. |
| Medication antidotes | Drugs like dexrazoxane, hyaluronidase, DMSO, or sodium thiosulfate may be used. |
| Temperature therapy | Cold or warm compresses help control the spread of the drug. |
Moving forward after extravasation
Experiencing extravasation during treatment can feel alarming, especially when you are already navigating cancer care. But in many cases, it is recognised early and managed quickly by trained medical teams.
Understanding the signs and symptoms of extravastion, and speaking up about any unusual sensations during an infusion can make a meaningful difference. With timely cancer treatment, clear extravasation management, and attentive monitoring, the focus remains on protecting tissue and keeping treatment as safe as possible.
FAQs
Related Blogs


Yeast Protein Supplement: A Nutritional Option for Cancer Patients