Leukopenia: Symptoms, Causes, and Treatment Explained
We don’t usually give much thought to white blood cells and what they do. But they quietly do their job every day, protecting the body, helping wounds heal, and keeping your immune system balanced. Life goes on, but a lower white blood cell count can shift that sense of normalcy into worry.
You might start asking questions like what does a low white blood cell count mean? Is leukopenia a cancer?
These thoughts are completely understandable.
This condition is usually referred to as leukopenia, a lower-than-normal number of white blood cells in the blood. Because these cells help the body fight infections, having fewer of them may make you more vulnerable to illness.
However, the encouraging part is that it’s not blood cancer, and healthcare specialists are very experienced in evaluating and managing this condition.
In this guide, we’ll walk through what leukopenia is, its symptoms, causes, leukopenia diagnosis, and treatment so you can feel more informed and supported about your health.
What is leukopenia?
Leukopenia means a shortage of white blood cells in the blood.
To understand leukopenia meaning, you must understand the role white blood cells (leukocytes) play in the body.
White blood cells help protect the body by:
- •Detecting harmful bacteria, viruses, and fungi
- •Attacking and destroying germs
- •Supporting healing and inflammation control
- •Coordinating the body’s immune response
Leukopenia is usually diagnosed when the total white blood cell count drops below about 4,500 cells per microliter of blood. This threshold is commonly referred to as the leukopenia range, although normal values can vary slightly depending on age, genetics, and overall health.
While you may develop mild leukopenia while recovering from a viral illness, it should resolve on its own as the immune system recovers.
However, in some cases leukopenia may be linked to serious conditions such as bone marrow disorders or cancer so oncologists may look for signs of cancer while determining the underlying cause.
Because white blood cells defend the body, low levels of them can increase the risk of infection, making it harder to fight even common germs.
However, leukopenia itself isn’t a disease but a diagnosis, so healthcare professionals focus on identifying the underlying cause to guide the right treatment and recovery plan.
4 types of leukopenia
When we talk about leukopenia, we are usually referring to a general drop in white blood cells. In some cases, these changes may also appear during cancer treatment, which is why oncologists often monitor white blood cell levels closely during care.
Because of this, oncologists often classify the leukopenia based on which type of white blood cell is affected. Below are the most common types of leukopenia that pathologists evaluate.
1. Neutropenia
Neutropenia occurs when your neutrophils, the most abundant white blood cells, are low. These cells are the immune system’s first responders against bacterial and fungal infections.
Because neutrophils are so important for early defence, neutropenia is the most common and often the most closely monitored form of leukopenia.
Pathologists often classify different grades of leukopenia based on how low the neutrophil count becomes.
2. Lymphocytopenia
Lymphocytopenia refers to a reduction in lymphocytes, which include T cells, B cells, and natural killer cells. These cells are responsible for your body to recognise viruses and produce antibodies.
Low lymphocyte levels may also appear during certain viral infections, autoimmune diseases, or immunosuppressant treatments.
3. Monocytopenia
Monocytopenia happens when monocytes fall below normal levels. Monocytes help remove damaged tissue and support healing during inflammation or infection.
Although less common than neutropenia, monocytopenia may sometimes occur in bone marrow disorders or after certain medical treatments.
4. Eosinopenia and Basopenia
These types of leukopenia occur when eosinophils or basophils are reduced. They are less commonly discussed because they often also fluctuate during stress, infections, or hormonal changes.
In most cases, we focus on the broader pattern of leukopenia rather than these rare changes alone.
Symptoms and causes of leukopenia
Initially, you may not feel anything unusual. Leukopenia itself often develops quietly and may only appear during a routine blood test. The symptoms usually begin when the body struggles to fight infections because there are fewer white blood cells available to protect it.
What are leukopenia symptoms?
When the immune system is weakened, the body may have trouble stopping germs that it would normally handle easily.
Some common signs of leukopenia include:
- Frequent infections
- Fever or chills
- Persistent cancer fatigue or weakness
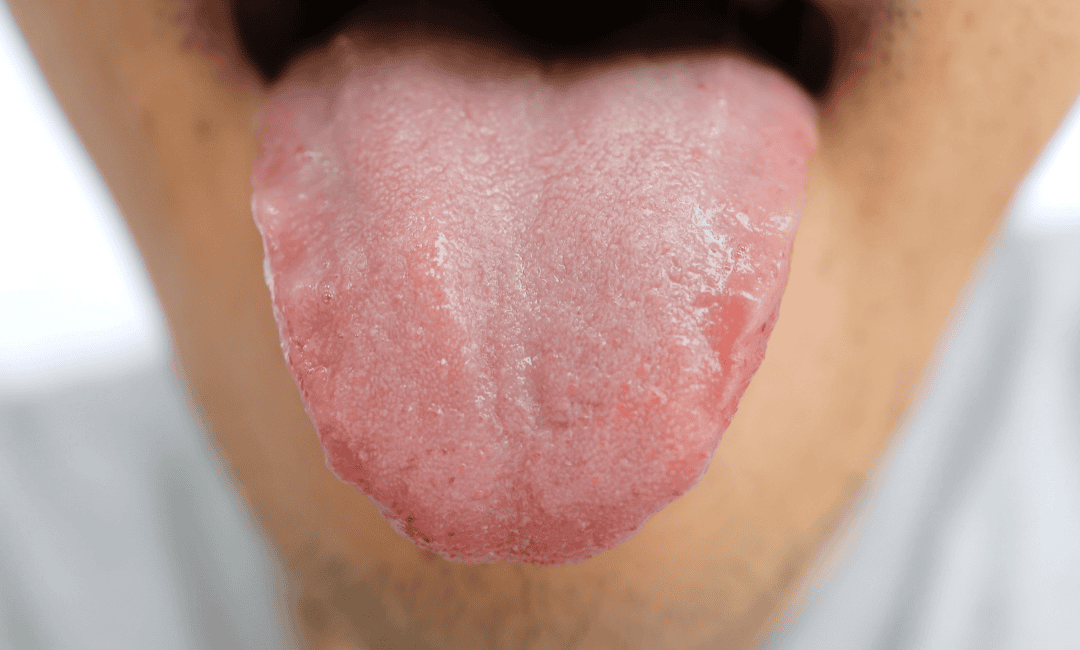
- Mouth ulcers or sore gums
- Slow-healing cuts or wounds
- Skin infections or rashes
- Sore throat or recurring respiratory infections
In more severe cases, infections may become more frequent or harder to treat. This is why oncologists also take potential leukopenia infection risks seriously for cancer patients.
Recognising these symptoms early can help prevent more serious leukopenia complications, especially in people with underlying health conditions.
What causes leukopenia?
Both short-term and severe medical conditions can lead to leukopenia. Here are a few frequent leukopenia causes:
| Possible cause | How can it lead to leukopenia |
|---|---|
| Viral infections | Certain viral illnesses can temporarily suppress bone marrow activity, reducing the number of white blood cells the body produces. |
| Cancer treatments | Chemotherapy and radiation therapy after cancer diagnostics can damage rapidly dividing cells in the bone marrow, which lowers white blood cell production. This is why oncologists closely monitor patients during leukopenia and cancer treatment. |
| Autoimmune disorders | Conditions such as lupus or rheumatoid arthritis may cause the immune system to mistakenly attack healthy white blood cells. |
| Bone marrow disorders | Cancer risk factors affecting the bone marrow can reduce or disrupt the production of white blood cells. |
| Medications | Some antibiotics, psychiatric medications, and anti-seizure drugs may occasionally lower white blood cell counts as leukopenia side effects. |
| Nutritional deficiencies | Low levels of nutrients such as vitamin B12, folate, or copper can interfere with healthy blood cell production. |
Diagnosis and tests
The diagnostic process for leukopenia is usually straightforward. A step-by-step approach is usually followed to understand whether the low white blood cell count is temporary, mild, or linked to another medical condition.
Complete blood count (CBC)
The first and most common test for leukopenia is a complete blood count (CBC). This blood test measures the total number of white blood cells along with other blood components like red blood cells and platelets.
It can also reveal if only one type of white blood cell is low or if several types are affected.
White blood cell differential
Your pathologist may also order a differential blood test, which measures the exact levels of each type of white blood cell. This helps identify patterns that may point to specific leukopenia conditions, such as neutropenia or lymphocytopenia.
Bone marrow examination
If the cause of leukopenia is unclear, a bone marrow aspiration or biopsy is usually ordered. This test examines the bone marrow, where blood cells are produced.
It allows specialists to see whether the marrow is producing enough healthy white blood cells or whether something, such as a bone marrow disorder or side effects of cancer, is affecting production.
Additional tests
Depending on the situation, doctors may also perform:
- •Infection screening for viruses or bacteria
- •Autoimmune tests to check for immune system disorders
- •Nutritional tests for vitamin B12, folate, or copper deficiencies
- •Medication reviews to see whether a drug may be affecting blood cell levels
Treatment options for leukopenia
The reassuring part is that leukopenia treatment usually focuses on addressing the underlying cause. Healthcare professionals usually tailor the management of leukopenia based on the severity of the condition and your overall health.
| Treatment approach | How it helps |
|---|---|
| Treating the underlying cause | Leukopenia can be caused by infections, autoimmune disorders, or nutritional deficiencies. Some types of cancer, such as leukemia and lymphoma, can also interfere with the body’s ability to produce healthy white blood cells. |
| Medications that stimulate white blood cell production | Growth factor medications may be used to encourage the bone marrow to produce more white blood cells, especially after chemotherapy or bone marrow suppression. |
| Infection management | If an infection develops, you might be prescribed antibiotics, antivirals, or antifungal medications to control it quickly. |
| Lifestyle precautions | Simple leukopenia precautions such as frequent hand washing, avoiding sick contacts, and proper wound care can help lower infection risk. |
| Monitoring and follow-up | In cases like mild leukopenia, doctors may recommend regular blood tests to monitor recovery. |
With proper care and monitoring, the leukopenia prognosis is often positive, especially when the condition is temporary or linked to a treatable cause.
Leukopenia and next steps
A diagnosis of leukopenia can feel worrying at first. But in many cases, leukopenia treatment is possible through finding the cause. If you notice possible leukopenia symptoms or receive abnormal blood test results, speak with a medical specialist. Early care can help protect your health and prevent complications.
If you or someone close to you has been diagnosed with leukopenia or is experiencing possible leukopenia symptoms, it’s important to speak with a medical specialist for palliative cancer care. Early evaluation and expert guidance can help determine the cause and create a care plan that supports your health moving forward.
FAQs
Related Blogs


Recognising the Signs of Cancer in the body that often go unnoticed