Guide to Mediastinal Tumour: Types, Symptoms & Causes
Learning that you have a mediastinal tumour can feel overwhelming. Because it develops near vital organs like the heart and lungs, it’s natural to feel scared or uncertain while trying to make sense of unfamiliar medical terms.
If you’re feeling anxious, know that many mediastinal tumours are benign (non-cancerous), and most can be effectively managed with modern medical care.
In fact, mediastinal tumours are usually discovered accidentally during a routine scan, and most people live perfectly normal lives after mediastinal tumour treatment.
This guide describes what a mediastinal tumour is, explains the types, and shows you the clear, advanced path toward healing.
What is a mediastinal tumour and where does it develop?
To understand the tumour, it’s critical to first understand the mediastinum. It is the space in the middle of your chest that holds multiple critical internal organs and mainly connects the two lungs.
A mediastinal tumour is simply an abnormal growth of cells that starts in this central space.
Because this area is so crowded, even a small mediastinal tumour can sometimes lean on a nerve or a blood vessel, which is often how they get noticed.
Mediastinal tumours classifications
The mediastinum is divided into three compartments. Knowing which compartment the tumour is in tells your oncologists exactly what kind of growth they are likely dealing with.
| Mediastinal compartment | Location | Description |
|---|---|---|
| Prevascular (anterior) compartment | Front of the chest, behind the breastbone (sternum) | The anterior part of the mediastinum is located between the sternum and the heart structures |
| Visceral (middle) compartment | Central area of the chest | Contains the heart, major blood vessels, trachea, and main airways |
| Paravertebral (posterior) compartment | Back of the chest, near the spine | Located alongside the vertebral column; contains structures related to nerves and the spine. |
Here are the three compartments discussed in more detail:
1. Anterior mediastinal tumour
This is the most common location for tumours in adults (about 50% of cases). You might find your oncologist referring to the "4 T's" when looking at this area:
- •Thymoma:A growth in the thymus gland. These are usually slow-growing.
- •Teratoma:A type of germ cell tumour that can actually contain different types of tissue, like hair or muscle (during development in the womb).
- •Thyroid:Sometimes the thyroid gland in the neck grows downward into the chest (a substernal goitre).
- •"Terrible" Lymphoma:This is a cancer of the lymph system. While the name is frightening, modern treatments for lymphoma are incredibly effective. Lymphoma differs from lung cancer because it arises from immune cells rather than lung tissue itself.
2. Middle mediastinal tumours
The most common middle mediastinal tumours are usually benign, such as pericardial cysts (near the heart). They are usually harmless but might be removed if they grow large enough to cause pressure.
Bronchogenic carcinoma (near the windpipe) can also sometimes extend into the mediastinum. So, it’s necessary to distinguish it from primary mediastinal growths.
3. Posterior mediastinal tumour
In children, this is the most common spot for mediastinal tumours. They usually start in the nerve tissues (neurogenic tumours). Most of these, like Schwannomas, are benign and easily treated, though some in infants can be more aggressive.
Rarely, tumours with similar symptoms may include a neuroendocrine tumour.
Although modern imaging focuses on three compartments, some older anatomical descriptions still refer to superior mediastinal tumours, which overlap mainly with anterior and middle compartment masses.
Symptoms and causes of mediastinal tumours
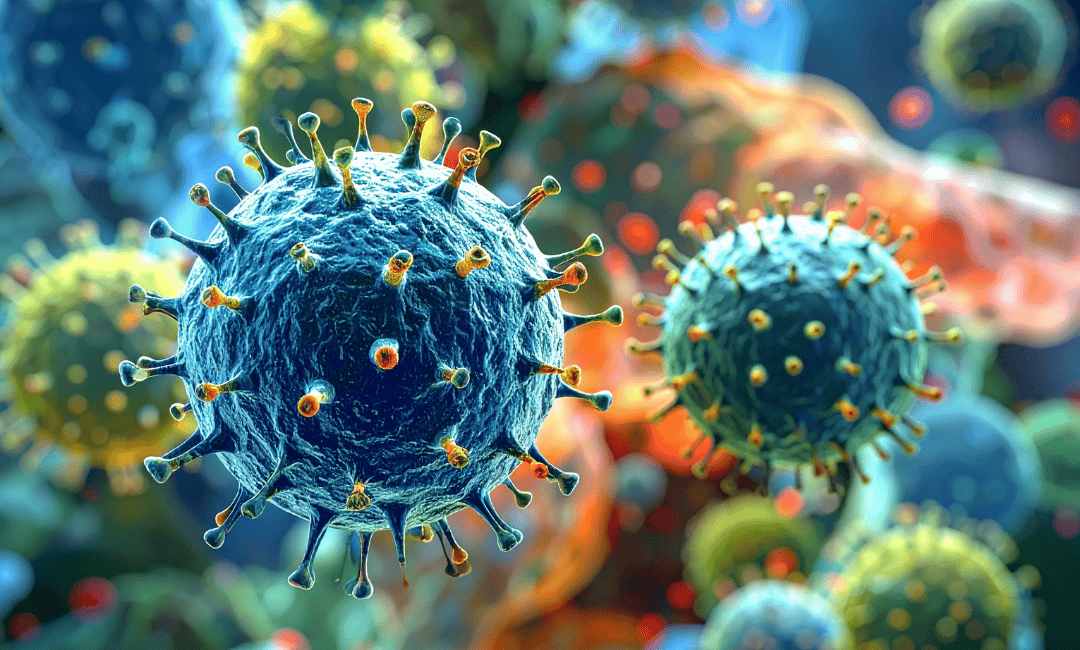
Roughly 40% of people have no symptoms of mediastinal tumours at all. Your tumour was likely found when you got a chest X-ray for a persistent cough or a minor injury. However, because the chest is a tight space, symptoms can occur when a mediastinal tumour starts "pushing" on other internal organs.
Mechanical symptoms (the "pressure" effect)
The symptoms originating from the pressure are:
- •Cough or Shortness of Breath
- •Puffiness in the face or neck
- •Hoarseness or Back Pain
- •Trouble Swallowing

Systemic symptoms
Some tumours are "biologically active." For example, 30–50% of people with a thymoma develop Myasthenia Gravis, a condition that causes muscle weakness, often starting in the eyes or face.
Causes and risk factors of mediastinal tumours
Despite common beliefs and unlike lung cancer, mediastinal tumours aren't usually linked to smoking. They often stem from:
- •Genetics:Certain conditions, such as Neurofibromatosis.
- •Developmental issues:Some cysts are present from birth, caused by tiny errors during embryonic growth.
- •Immune System issues:Since the thymus gland produces your immune cells, sometimes it can produce abnormal growths.
Diagnosis of mediastinal tumours
If your pathologist suspects a tumour, they may use non-invasive imaging techniques first to diagnose the tumour growth:
| Imaging test | What it does | What pathologists learn |
|---|---|---|
| CT scan | Detailed cross-sectional chest images | Shows tumour size, exact location, and whether it touches blood vessels or airways; can detect fat or calcification |
| MRI | High-detail soft tissue imaging | Helps evaluate posterior tumours and tells solid tissue apart from fluid-filled cysts. Chemical-shift MRI is particularly useful for differentiating thymic hyperplasia from a malignant neoplasm. |
| PET scan (PET-CT) | Measures cell activity using a small amount of radioactive sugar | Helps distinguish benign growths from aggressive cancers and is important for lymphoma staging |
Imaging also helps distinguish superior mediastinal tumours from masses arising lower in the chest.
If your tests are still not conclusive about benign and malignant tumours, you might be asked to undergo a biopsy. The type of biopsy you’re gonna get will depend on the location and type of your mediastinal tumour. Some of the more invasive procedures to confirm the diagnosis are:
- •EBUS-TBNA (Endobronchial Ultrasound)
- •Mediastinoscopy
- •Chamberlain Procedure
- •CT-Guided Needle Biopsy
Mediastinal tumour staging
Mediastinal tumour staging is used to describe the stages of cancer. This helps oncologists to know how fast your mediastinal tumour is growing.
For many years, pathologists used the Masaoka-Koga system, which looked at whether the tumour had broken through its "capsule" (like the skin of a grape). The technology has now moved toward the TNM system, which is more precise.
The 9th Edition update even looks at tumour size. If a tumour is under 5 cm, it's categorised differently from one over 5 cm. This allows oncologists to be much more specific with their treatment plans rather than using a one-size-fits-all approach.
Here is a quick overview of what the tumour stagings mean:
| Stage | What it means |
|---|---|
| Stage I | The tumour is contained within its "shell" or the nearby fat. Highly treatable. |
| Stage II/III | The tumour has started to grow into nearby organs (like the heart lining). |
| Stage IV | The tumour has spread to more distant parts of the chest or other organs. |
Mediastinal tumour treatment options
The goal of mediastinal tumour treatment is always to remove or shrink the growth while protecting your vital organs.
Modern mediastinal tumour surgery
The surgeries have moved from sternotomy (opening the breastbone) to VATS and robotic surgery.
Most mediastinal tumour surgery procedures now use tiny incisions and robotic arms (like the Da Vinci system) to remove tumours. This means less pain, smaller scars, and a much faster recovery.
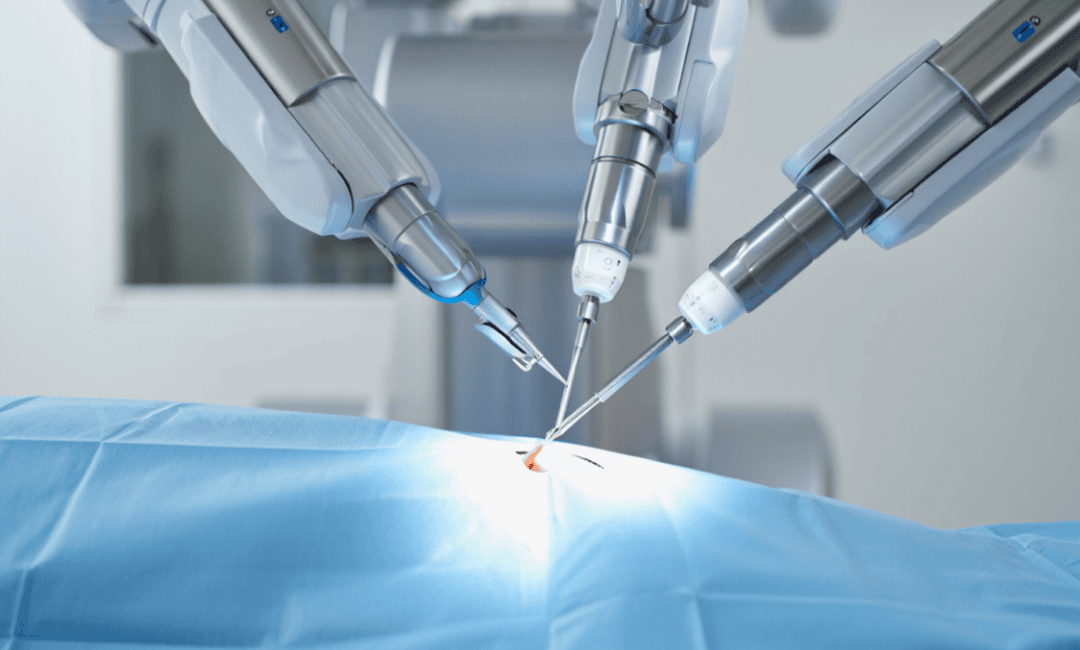
Targeted therapies
For more aggressive tumours, oncologists no longer just rely on standard chemotherapy. Immunotherapy helps your own immune system find and eliminate the cancer cells. This has been helpful for cases that were once considered difficult to treat.
Radiation
Precise beams of energy can be used to clean up any microscopic cells left behind after surgery, ensuring the tumour doesn't come back.
Living well after diagnosis
A mediastinal tumour diagnosis can feel frightening. But it is important to remember that most of these growths are benign, and malignant tumours are highly treatable. The mediastinal tumour survival rate is also excellent when diagnosed early. Modern imaging, precise staging, and minimally invasive treatments allow oncologists to plan care safely and effectively.
With early evaluation and the right cancer treatment approach, most patients recover well and return to their normal routines. You are not expected to navigate this journey alone.
Clear guidance, experienced care, and compassionate support can make each step more manageable, helping you move forward with confidence, reassurance, and hope.
FAQs
Related Blogs


Recognising the Signs of Cancer in the body that often go unnoticed