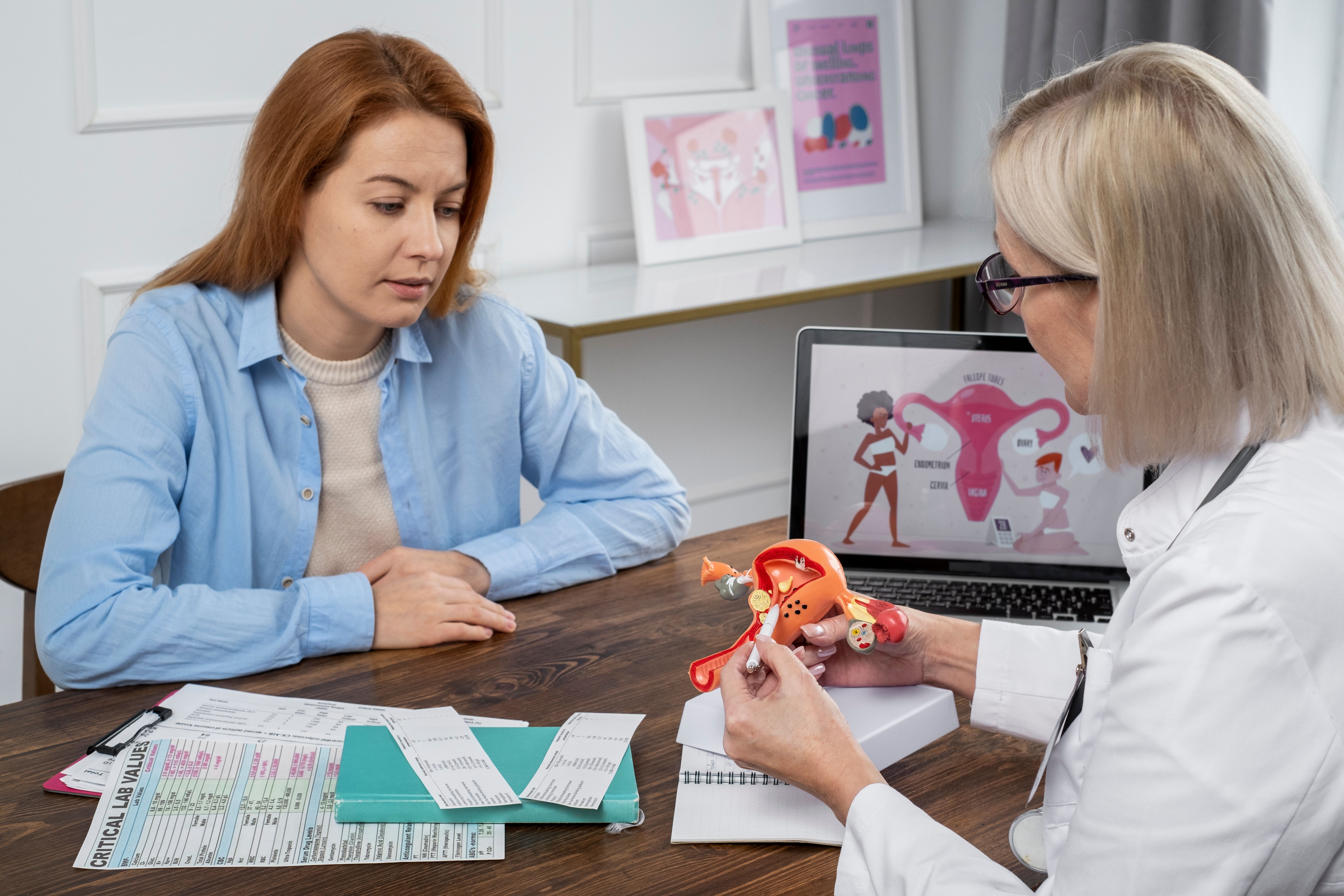
What is Myelofibrosis? Causes, Symptoms, and Treatment Options
A diagnosis of myelofibrosis can turn anyone's world upside down. The word itself sounds intimidating, but behind that complex name is a condition that can be managed with the right care and support.
Thousands of people around the world are living with myelofibrosis and living well. Medical science is advancing faster than ever, treatment options are growing, and doctors today understand this condition better than they ever have before.
What you can do for yourself or for your loved one is be aware of the condition. It will help regain control and take the right steps forward.
In this guide, we'll walk you through all you need to know about myelofibrosis meaning, causes, diagnosis, and treatments that can help.
What is myelofibrosis?
Myelofibrosis is a kind of bone marrow disorder or blood cancer that makes it difficult to make blood cells. It belongs to a group of cancers called myeloproliferative neoplasms.
Your bone marrow is the spongy tissue inside your bones responsible for producing blood cells. When it gets scarred, it cannot normally make red blood cells, white blood cells, and platelets.
Over time, the body tries to compensate by producing blood cells in other organs, particularly the spleen and liver - causing them to enlarge. It progresses slowly in most cases, but its impact on quality of life can be huge if not promptly monitored.
But don't worry, just staying in continuous touch with your care team for yourself or your loved one can be enough to manage the condition well.
Types of myelofibrosis
Myelofibrosis classification is based on whether the disease develops on its own or from another condition. Understanding this difference matters for cancer treatment planning and outlook.
- •Primary myelofibrosis (PMF):This form develops on its own, without an underlying blood disorder. It is the most common type and arises from a genetic mutation in bone marrow stem cells.
- •Secondary myelofibrosis:This develops as a progression from another blood condition, most commonly polycythemia vera or essential thrombocythemia. It behaves similarly to primary myelofibrosis but has a different origin point.
Besides these two primary types, acute myelofibrosis is a rare and rapidly progressing form that involves a sudden decline in blood cell production and requires immediate medical attention.
However, this condition takes time to develop, so you can with prompt care and timely treatment avoid your myelofibrosis from worsening.
Autoimmune myelofibrosis is an uncommon variant. In this, the immune system mistakenly attacks bone marrow tissue, triggering fibrosis. It may respond differently to standard treatments.
What are the symptoms of myelofibrosis?
Myelofibrosis symptoms often develop gradually, which means many people live with the condition for months before receiving a diagnosis. Some people have no symptoms at all in the early stages.

When symptoms do appear, they can range from mild fatigue to greater physical changes that affect daily life. Here are the most common myelofibrosis symptoms:
- •Fatigue and weakness due to anaemia
- •Shortness of breath, especially during physical activity
- •An enlarged spleen causing discomfort or fullness under the left rib
- •Night sweats and low-grade fever
- •Unexplained weight loss
- •Easy bruising or bleeding
- •Pale skin
- •Bone or joint pain
- •A sensation of itching (sometimes called cancer itching) linked to abnormal cell activity
- •Feeling full quickly when eating
These symptoms often overlap with other conditions, which is why careful medical evaluation is so important.
What causes the condition?
Myelofibrosis causes isn't fully understood yet, but researchers have traced it back to changes in the DNA of blood stem cells in the bone marrow.
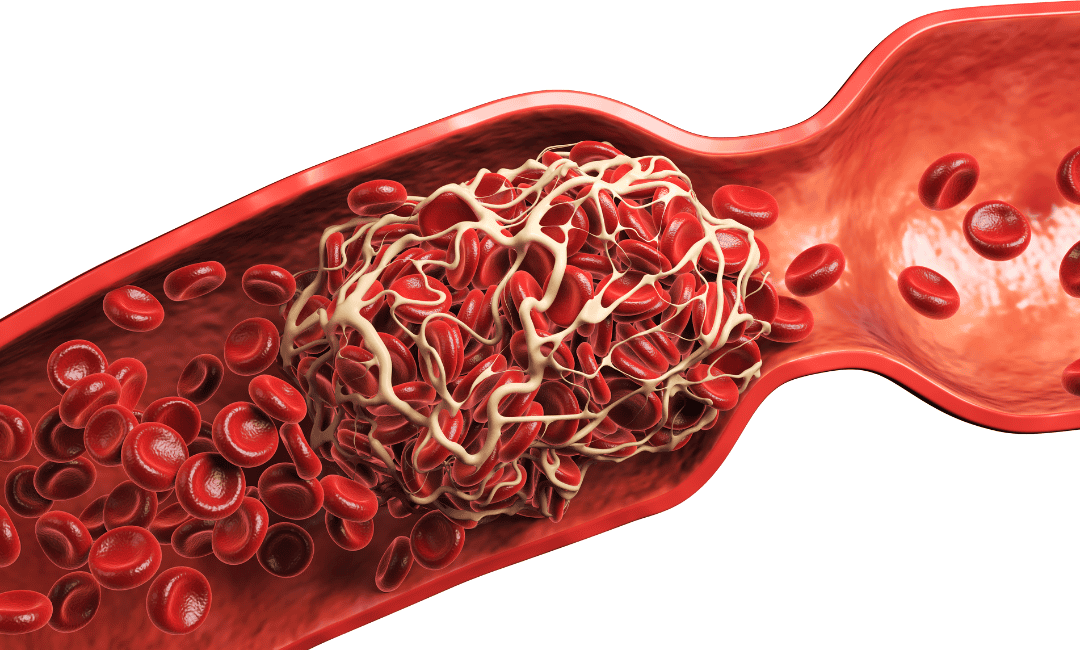
Normally, a cell's DNA acts like an instruction manual, telling it exactly what to do. In myelofibrosis, those instructions get altered, causing blood stem cells to produce more blood cells than the body actually needs.
Over the years, medical researchers have identified a few specific genetic changes that can lead to this condition.
- JAK2 gene mutation is the most common factor responsible. This genetic mutation cancer link is well established - it causes blood stem cells to grow and divide without normal checks.
- The CALR gene mutation affects a protein involved in how cells handle stress and fold properly. When this gene is mutated, it activates the same signalling pathway as JAK2. Patients with this mutation tend to have a somewhat better myelofibrosis prognosis compared to those with JAK2.
- MPL gene mutation affects a protein called the thrombopoietin receptor, which plays a role in regulating platelet production. When this gene changes, it drives abnormal cell growth and contributes to fibrosis.
Diagnosis and tests
Since the symptoms of this condition can overlap with other medical disorders, your doctors use a combination of tests and careful myelofibrosis grading to confirm the condition and assess its severity.
While the idea of cancer diagnostics tests can feel overwhelming, these are routine procedures that doctors perform regularly to get a clear picture of your health. In most cases, these tests simply help rule out possibilities and guide your care in the right direction.
1. Physical exam and blood tests
Your doctor will begin by asking about your symptoms and gently examining your abdomen to check whether the spleen or liver shows any signs of swelling. This cancer screening test approach is usually the very first step in evaluation.
Based on what they find, they may recommend blood tests to look for any unusual changes in your cell counts.
2. Imaging tests
To get a closer look, your doctor may suggest an ultrasound or an MRI scan. These help measure the size of your spleen and liver, making it easier to understand how the condition may be affecting your organs.
They're also useful for tracking any changes over time and can pick up on blood clots or vascular concerns that sometimes accompany this condition.
3. Bone marrow biopsy
A biopsy is the most reliable way to confirm a diagnosis. During this procedure, a small sample of marrow is collected from the hip bone and examined under a microscope.
The degree of fibrosis is then graded on a scale from MF-0 to MF-3, which helps your doctor understand how much scarring is present and what stage the condition is at. It shapes your personalised treatment plan and helps determine whether you fall into low risk myelofibrosis or high risk myelofibrosis categories.
Treatment and management of myelofibrosis
Myelofibrosis treatment depends on several factors, including your risk category, age, overall health, and myelofibrosis stages.
If you fall into a low-risk group and aren't experiencing any symptoms, you may not need treatment right away. In that case, your doctor will monitor your health closely and watch for any changes before deciding on the next steps.
When treatment is needed, the options typically include myelofibrosis medications medications, therapy, and in some cases, a transplant. The goal across all of these is to relieve symptoms, slow disease myelofibrosis progression, and help you maintain a good quality of life.
1. JAK inhibitor therapy
JAK inhibitors like ruxolitinib and fedratinib are the most commonly used medications for myelofibrosis today. They work by targeting the overactive JAK-STAT signalling pathway that drives the disease, which helps reduce spleen size and ease symptoms like fatigue and night sweats.
This is the cornerstone of primary myelofibrosis treatment for intermediate and high-risk patients.
2. Stem cell transplant
An allogeneic stem cell transplant is currently the only known cure for myelofibrosis. The procedure involves replacing diseased bone marrow with healthy donor cells and is generally considered for younger patients with high-risk disease who have a suitable donor match.
While it does carry risks such as graft-versus-host disease, it can offer the possibility of long-term remission for the right candidates.
3. Supportive care
Supportive care is all about managing symptoms and helping you feel your best through the course of treatment. This can include blood transfusions for severe anaemia, growth factors to boost blood cell production, and medications to address bone pain or itching.
In addition, it can cover nutritional support, gentle exercise, and mental health resources to support your overall well-being.
Hope, awareness, and the right care can change everything!
Receiving a myelofibrosis diagnosis can feel overwhelming, but you're not alone in this, and there is real reason for hope.
Many new drug combinations like BET inhibitors and PI3K inhibitors are being studied in clinical trials, with some targeting specific mutations and others focusing on the bone marrow microenvironment.
Targeted therapies are also available to help keep symptoms in check so the condition doesn't get in the way of your everyday life. And for those who qualify, curative options do exist.
The best thing you can do right now is understand your condition or that of your loved ones. Know the risk category, mutation status, and the treatment paths available.
At Everhope, our team of specialists is here to answer your questions and help you find the care that's right for you. With the right support, a fulfilling life after diagnosis is absolutely within reach.
FAQs
Related Blogs


Recognising the Signs of Cancer in the body that often go unnoticed