
Immune System and Cancer: Understanding the Defence Process

Perhaps you've heard people say that a strong immune system prevents cancer. Or maybe your doctor mentioned that your white blood cell counts are low during treatment, and you need to be careful about infections.
These conversations raise important questions about the connection between immunity and cancer that many patients struggle to understand clearly.
How exactly does your body recognise cancer cells amongst the trillions of normal cells? Why does chemotherapy that's meant to fight cancer actually weaken your immune defences? And can you truly boost your immunity to help fight cancer more effectively?
Understanding the relationship between the immune system and cancer helps you make sense of what's happening in your body, and what you can realistically do to support your immune health.
What is the role of the immune system in cancer?
The role of immune system in cancer extends far beyond fighting infections to include constant surveillance for abnormal cells that could become cancerous.
Every day, your cells divide trillions of times to replace old or damaged tissues. During constant replication, mistakes occur. There can be DNA copying errors, environmental exposures, or random mutations that create abnormal cells with precancerous characteristics.
Your immune system continuously surveils, identifying and eliminating abnormal cells before they can multiply into tumours. This process, called immunosurveillance, represents your body's first line of defence against cancer development.

3 Es of cancer immunoediting
Scientists describe the immune system against cancer through three phases called the 3 Es:
- 1. Elimination: Early abnormal cells are recognised and destroyed before becoming problematic. This represents successful immune surveillance working as intended.
- 2. Equilibrium: Some abnormal cells survive initial elimination, but immune responses keep them controlled, preventing growth into detectable cancer. This dormant state can last years or decades.
- 3. Escape: Eventually, some cancer cells acquire mutations allowing them to evade immune detection or suppress immune responses, leading to tumour growth.
Understanding this progression helps explain why cancer risk factors that weaken immunity (chronic stress, poor nutrition, lack of sleep) increase cancer development risk over time.
How does the immune system recognise cancer cells?
The mechanism of how does immune system recognises cancer cells involves detecting molecular differences that distinguish cancerous cells from healthy ones.
Cancer cells display abnormal proteins on their surfaces called tumour antigens, which serve as identification tags that immune cells can recognise. These antigens arise from genetic mutations, viral proteins (in virus-associated cancers), or abnormal expression of proteins normally present only during fetal development.
Types of cancer-identifying markers:
- •Mutated proteins:Genetic changes create proteins never seen before in the body
- •Overexpressed proteins:Normal proteins produced in excessive amounts
- •Cancer-testis antigens:Proteins normally found only in reproductive tissues are inappropriately expressed by tumours
- •Viral antigens:Proteins from cancer-causing viruses like HPV or Epstein-Barr virus
How does immune system recognise cancer cells specifically occurs through pattern recognition receptors on immune cells that detect danger signals and abnormal molecular patterns.
When cells become stressed, damaged, or transformed into cancer, they release distress signals that alert immune cells.
However, this recognition pattern can fail sometimes. This explains why boosting immune system to fight cancer doesn't guarantee prevention, as it can be outsmarted by sufficiently evolved cancer cells.
Cancer patient immune system: What changes during treatment?
Even before treatment begins, cancer can weaken immune function through several mechanisms:
- Direct immune suppression: Tumours produce substances that actively suppress immune cell function, creating local and sometimes systemic immunosuppression. This helps cancer evade destruction.
- Bone marrow infiltration: Blood cancers or metastases to bone marrow reduce the production of immune cells, lowering white blood cell counts.
- Nutritional depletion: Cancer's high metabolic demands and effects on appetite lead to malnutrition, which impairs immune function significantly.
- Inflammation: Chronic inflammation from cancer paradoxically suppresses effective immune responses while creating conditions favouring tumour growth.
- Paraneoplastic syndromes: Some cancers trigger immune responses that mistakenly attack normal tissues, depleting immune resources.
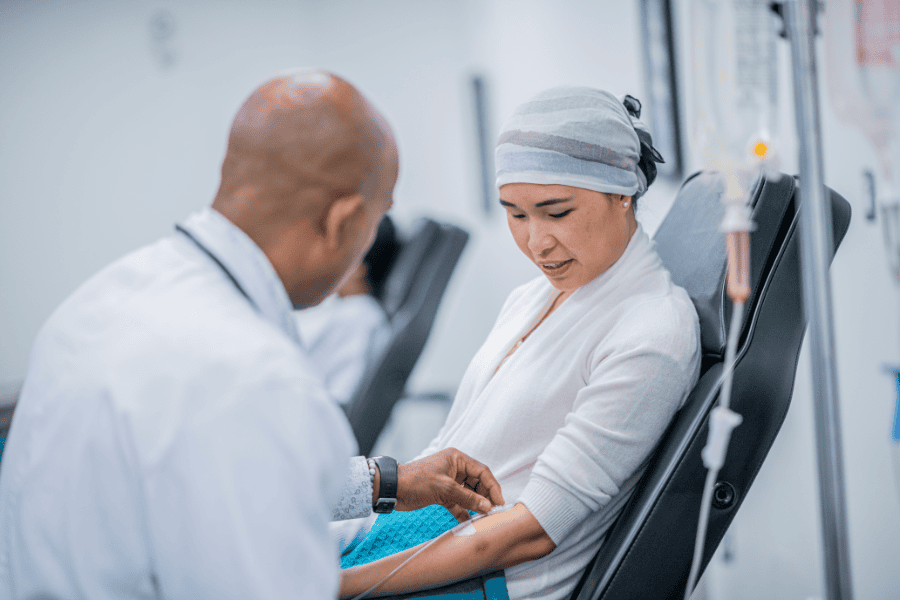
Chemotherapy and immunity
Chemotherapy drugs target rapidly dividing cells, which unfortunately include immune cells in bone marrow and lymph nodes alongside cancer cells.
Immune effects of chemotherapy include:
- •Neutropenia:Dramatically reduced neutrophils (infection-fighting white blood cells)
- •Lymphopenia:Decreased lymphocytes, including T cells and B cells
- •Impaired antibody production:Reduced ability to respond to infections
- •Mucositis:Damaged gut and mouth linings allow bacteria to enter the bloodstream
Radiation therapy effects on immune system and cancer
Radiation therapy affects immunity less systemically than chemotherapy but creates local immune suppression in treated areas.
Large radiation fields (whole abdomen, extensive bone marrow areas) can reduce blood cell production substantially.
Understanding these changes helps explain why infection prevention measures (hand hygiene, avoiding crowds during neutropenic periods, prompt fever evaluation) matter tremendously during cancer treatment.
Can a weak immune system cause cancer?
The question "can a weak immune system cause cancer" requires a nuanced understanding of how immune deficiency influences cancer risk.
People with severely compromised immune systems develop cancer at dramatically higher rates than the general population, providing clear evidence that immunity matters for cancer prevention.
High cancer rates occur in:
- •HIV/AIDS patients (before effective antiviral treatment)
- •Organ transplant recipients taking immunosuppressive drugs
- •People with inherited immune deficiencies
- •Patients on long-term immunosuppressive medications for autoimmune diseases
However, the cancers these populations develop aren't typical solid tumours but primarily virus-associated cancers (Kaposi sarcoma, lymphomas, cervical cancer) and blood cancers.
Common cancers like breast, prostate, or lung cancer don't increase dramatically with immune suppression.
So, does cancer weaken the immune system? Yes, as discussed. But can a weak immune system cause cancer directly? The relationship is more complex than simple causation.
Immune deficiency contributes to cancer through:
- •Reduced surveillance, allowing precancerous cells to accumulate
- •Inability to control cancer-causing viruses (HPV, EBV, HHV-8)
- •Chronic inflammation from recurrent infections
- •Impaired DNA repair mechanisms
However, most common cancers develop from what causes cancer factors like genetic mutations, environmental exposures (smoking, radiation), hormonal influences, and ageing, rather than simple immune weakness.
Strong immune system and cancer: Why immunity matters
Understanding the connection between a strong immune system and cancer helps clarify realistic expectations about what immune health can and can't accomplish.
- •Better treatment tolerance:Patients entering treatment with good immune function generally tolerate chemotherapy better, experience fewer dose delays, and maintain better quality of life.
- •Faster recovery:Strong baseline immunity supports quicker recovery of blood counts after each treatment cycle.
- •Reduced infection risk:Better immune function means fewer serious infections during vulnerable treatment periods.
- •Potentially better outcomes:Some research suggests robust immunity at diagnosis correlates with better cancer survival, though multiple factors confound this relationship.
- •Improved vaccine responses:Better ability to respond to vaccines, including flu, pneumonia, and COVID-19 vaccines that protect during treatment.
A strong immune system and cancer prevention connection exists but it isn't absolute. Many people with excellent immune health develop cancer, while some with compromised immunity never do.
Strengthening immune system to fight cancer
Evidence-based approaches to strengthening the immune system focus on supporting natural immune function through lifestyle and medical interventions.
Oncology nutrition for immune support emphasises adequate protein, micronutrients, and overall calorie intake rather than specific "superfoods."
Diet for cancer patients supporting immunity includes:
- •Adequate protein:1.2-1.5 grams per kilogram body weight daily supports white blood cell production
- •Colourful vegetables and fruits:Provide antioxidants and phytonutrients supporting immune cell function
- •Zinc-rich foods:Shellfish, meat, beans, nuts support T cell development
- •Vitamin D:Adequate levels support immune regulation (supplement if deficient)
- •Probiotics:Fermented foods support the gut microbiome, which is crucial for immune function
- •Hydration:Adequate fluids support lymphatic system function
Moreover, exercise for cancer patients supports immune function through multiple mechanisms, including improved circulation distributing immune cells throughout the body, reduced inflammation, and improved sleep supporting immune recovery.
Also, there are benefits of stretching and yoga for cancer patients, which help in reducing stress. These tips, along with complete and sound sleep, can act as an immune system booster for cancer patients.
Conclusion on the immune system and cancer cells
The intricate connection between your immune system and cancer involves constant surveillance, recognition, and elimination of abnormal cells that arise naturally throughout life.
When this system works optimally, it prevents countless potential cancers from ever developing into detectable disease. Yet the cancer patient immune system faces unique challenges from both disease and treatment, requiring thoughtful support and protection.
Your immune system represents a powerful ally in your cancer journey, deserving support through healthy lifestyle choices, while recognising it works best in partnership with evidence-based medical care.
For comprehensive cancer care that integrates immune support strategies, nutritional guidance, and evidence-based treatments, connect with experienced oncology specialists at Everhope, who can provide personalised recommendations to support you throughout treatment and recovery.
FAQs
Related Blogs


ZMA Supplements: Benefits for Cancer Recovery, Sleep & Immunity


