Understanding Viruses That Cause Cancer and How You Can Protect Your Health
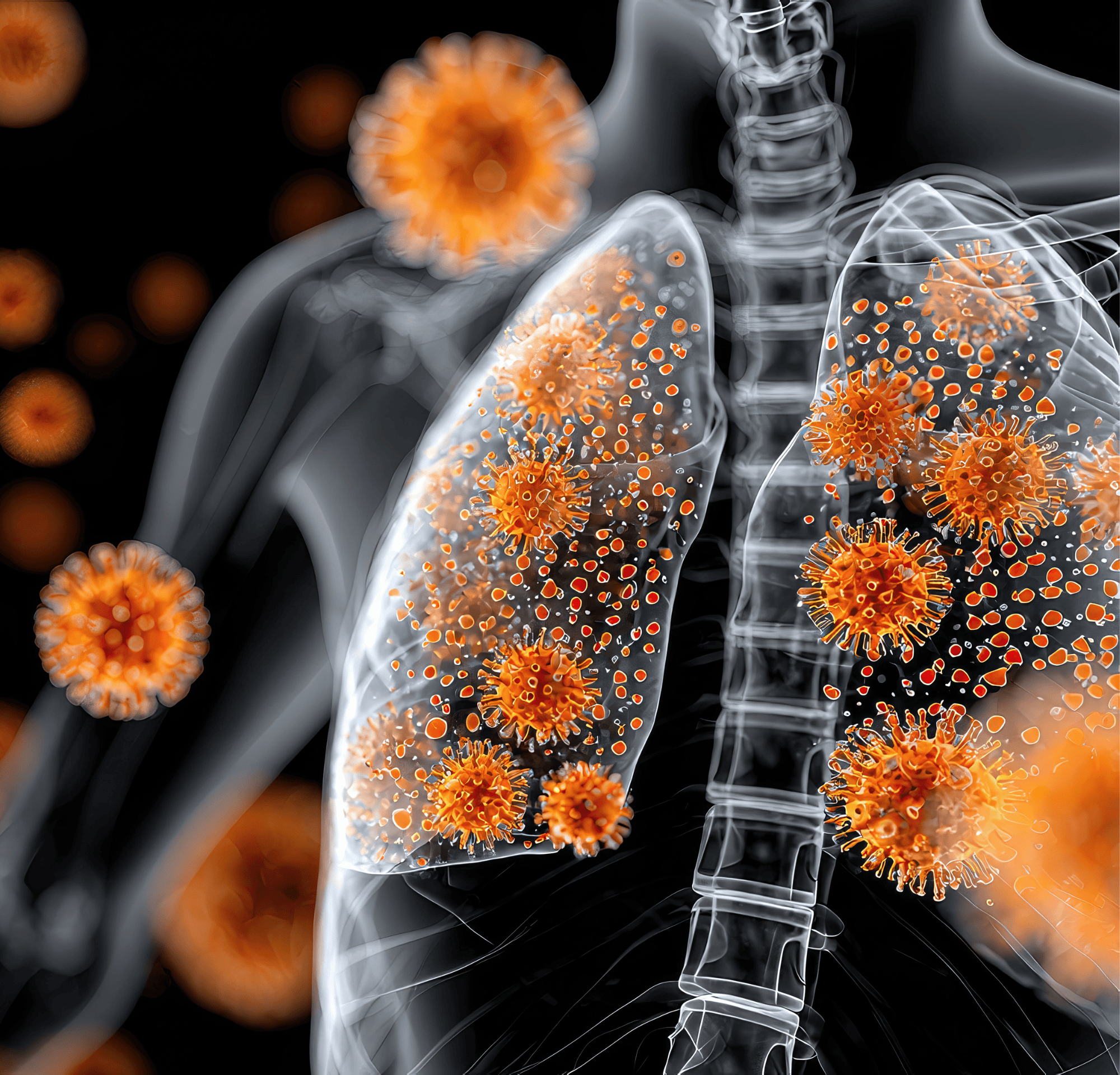
Hearing that viruses can be linked to cancer may feel unsettling, especially when viruses are usually associated with short-lived illnesses like a cold or the flu. You are not alone in wondering what this means for your health, and reliable information can help you feel more in control.
Not every viral infection leads to cancer, and only certain viruses that cause cancer change how cells behave over time. These cancer causing viruses are known as oncogenic viruses.
In this article, we’ll explore how viruses and cancer are connected and explain the main viruses that cause cancer, along with practical steps you can take to protect yourself.
Viruses and cancer: Understanding the connection
To understand how viruses cause cancer, think of your cells as a highly regulated factory. Usually, there are tumour suppressor proteins that stop the assembly line if a mistake is made.
Oncogenic viruses enter the cells and do one of two things:
- 1. Direct Sabotage:Cancer causing viruses have genes called oncogenes that override normal cell controls. They insert into your DNA, producing oncoproteins. It forces the cells to divide uncontrollably.
- 2. Chronic Inflammation:They create a state of constant red alert in the body. This persistent irritation causes long-term damage to the surrounding tissue, turning healthy cells into tumours.
But having one of these viruses does not mean cancer is inevitable. Here’s what viruses cause cancer and how to prevent them.
Human papillomavirus (HPV): The most preventable cancer risk
Human papillomavirus (HPV) is arguably the most well-known virus in this category and one of the most common viruses that cause cancer worldwide. It’s the primary driver of cervical and anogenital cancers globally.
HPV and cervical cancer
Almost all cervical cancer symptoms and cases are linked to high-risk strains of HPV, specifically HPV-16 and HPV-18. These strains produce two aggressive proteins, E6 and E7.
- •E6destroys the p53 protein, which normally tells a damaged cell to self-destruct for the safety of the body.
- •E7disables the Rb protein, which acts as a brake on cell growth. Without these brakes, your cells can grow without end.
HPV and other cancers
HPV infection doesn’t stop at the cervix. It is increasingly responsible for head and neck cancers (HNSCC), particularly in men. Interestingly, lifestyle factors like tobacco use act as a multiplier.
Tobacco smoke actively tells the HPV virus to produce more cancer-causing proteins, creating a perfect environment for tumour growth.
HPV vaccination and cancer prevention
The HPV vaccine is essentially a cancer-prevention shot. Women who were vaccinated had a staggering reduction in cervical cancer compared to those who weren't.
Global health organisations are now moving toward a single-dose regimen, making it easier and cheaper for people everywhere to get protected.
Epstein-Barr virus (EBV)
Most people know EBV as the cause of mono (infectious mononucleosis), but it is also among the important viruses that cause cancer in certain populations.
While you can carry EBV for life without issue, for some, it can lead to Burkitt’s lymphoma or nasopharyngeal (nose and throat) cancer.
EBV hides inside your B-cells as a tiny circle of DNA called an episome. It doesn't always integrate into your DNA; instead, it floats nearby and manipulates how your genes are expressed.
EBV also often teams up with Malaria. The constant immunity engagement from malaria wakes up the EBV, causing B-cells to multiply so rapidly that a cancerous mutation becomes almost inevitable.
Hepatitis B virus (HBV) and Hepatitis C virus (HCV)
These two viruses are the leading causes of liver cancer (hepatocellular carcinoma) and are major viruses that cause cancer affecting the liver globally.
- •HBV is a DNA virus that physically weaves itself into your liver cell's blueprint.
- •HCV is an RNA virus that causes so much chronic inflammation and scarring (cirrhosis) that cancer eventually takes root.
While oncology is getting better at treating Hepatitis with vaccines and antivirals, the fatty liver disease (MASLD) is starting to overtake viruses as the leading cause of liver cancer.
Human immunodeficiency virus (HIV) and cancer risk
In contrast to the other viruses mentioned, HIV does not directly cause cancer by changing cell DNA, but it increases vulnerability to other viruses that cause cancer.
By depleting the body’s T-cells, HIV leaves your body’s immune system weaker. When your immune system is weak, other viruses like HPV or EBV can attack.
This is why people living with HIV have much higher rates of Kaposi’s sarcoma and certain lymphomas.
Fortunately, modern antiretroviral therapy (HAART) helps keep the immune system strong enough to prevent many of these secondary cancers.
Human Herpesvirus 8 (HHV-8)
HHV-8 is the primary cause of Kaposi’s Sarcoma (KS) and is one of the rarer viruses that cause cancer in humans. It causes purple or red spots on the skin or inside the mouth.
HHV-8 forces the host cell to change how it uses sugar and oxygen, creating an environment that fuels rapid tumour growth and the formation of new, leaky blood vessels.
Human T-lymphotropic virus type 1 (HTLV-1)
HTLV-1 was the first human retrovirus ever discovered and remains one of the unique viruses that cause cancer through long-term cellular transformation. It causes a very aggressive form of leukaemia.
Unlike HIV, which kills the cells it infects, HTLV-1 makes them immortal.
It spreads through what is basically a bridge between cells, where the immune system can’t see it. Because it stays hidden for decades, you may not even know they have it until a malignancy develops later in life.
Merkel cell polyomavirus (MCV)
MCV is linked to a rare but very aggressive skin cancer and represents one of the newly identified viruses that cause cancer.
What makes this cancer unique is how it responds to treatment. It is a very simple cancer with few mutations and highly visible to the immune system.
This makes it a prime candidate for immunotherapy, where we use the body's own T-cells to hunt down the virus-infected cancer cells.
Who is at higher risk of virus induced cancer?
The jump from a simple infection to virus induced cancer doesn't happen to everyone. The cancer risk factors include:
- •Immune Suppression: Whether from HIV, organ transplant meds, or genetics.
- •Lifestyle Factors: Smoking and alcohol accelerate viral oncogenesis.
- •Dietary Toxins: In some parts, a mould called Aflatoxin (found in poorly stored grain) works with Hepatitis B to cause rapid liver cancer.
- •Co-infections: Having two viruses (like HIV and HPV) at once significantly raises the risk.

How can virus-induced cancer be prevented?
A common misconception is that all cancers are caused by viruses, but infections are responsible for only a fraction of cancer cases worldwide. The good news is that the viruses that cause cancer are among the most researched diseases.
Vaccination
Vaccination for viruses that cause cancer is one of the most effective public health strategies today.
The Hepatitis B vaccine is essentially named the world's first cancer vaccine. Similarly, the HPV vaccine can prevent over 90% of related cancers if given early.
Early detection and screening
If we can't prevent the infection, we can catch the pre-cancer early.
- Cervical Screening: Early HPV cervical cancer screening helps detect changes caused by viruses that cause cancer before tumours develop. Pathologists now prefer primary HPV testing every 5 years over the traditional Pap smear. Many clinics even offer self-collection kits, which are just as accurate and much more private.
- Liver Monitoring: For those with chronic Hepatitis, regular ultrasounds and blood tests (like the AFP test) are vital.
Safe lifestyle and infection control
Because many of these viruses are shared through blood or intimate contact, barrier protection and needle safety remain pillars of prevention.
Furthermore, smoking cessation and limiting alcohol are the best ways to starve a latent virus of the triggers it needs to turn into cancer. Healthy habits reduce the long-term effects of viruses that cause cancer on the body.
Moving forward with hope
Many people ask, is cancer a virus, before learning how infections and cancer are actually connected. The connection between viruses and cancer is deep, but it doesn't have to be a source of fear.
Many virus-related cancers are now among the most preventable forms of cancer, thanks to vaccines, regular screenings, oncology doctors, and advances in cancer treatment that support your body’s natural defences. By staying informed and leaning into preventative care, you are taking active, loving steps to protect your and your loved ones' future.
FAQs
Related Blogs