Kaposi Sarcoma: Types, Symptoms, and Treatment

Most people don’t go looking for information about Kaposi sarcoma. It usually enters the picture unexpectedly: a note on a report, a comment during an appointment, or a skin change that lingers longer than expected. When a name you’ve never heard before suddenly matters, it’s normal for the mind to jump ahead before the facts catch up. It’s important to know, this illness follows its own rhythm. Some forms move slowly, others need closer attention, and many respond well when recognised early.
Knowing how it develops, how symptoms can appear, and how care is approached brings the situation into sharper focus - exactly what we cover below! With clarity comes steadier footing, and a clearer sense of the road ahead.
What is Kaposi sarcoma?
Kaposi sarcoma definition refers to it as a soft tissue sarcoma, meaning it develops from connective tissues such as blood and lymph vessels rather than from solid organs.
Unlike other tumours, Kaposi sarcoma cancer often shows itself on the skin before affecting deeper tissues. Those tell-tale kaposi’s sarcoma lesions may appear as flat or raised patches on the skin, though the disease can also involve internal organs over time.
This disease is not a single experience; it unfolds differently in each person, depending on immune function, viral triggers, and how far it has progressed.
Types of Kaposi sarcoma
Thick family history and genetics don’t define this condition; instead, the context around the immune system does. There are several types of it, and each tells a slightly different story:
- 1. Epidemic (AIDS-related): Often referred to as Kaposi sarcoma AIDS, this form is most commonly seen in people living with HIV, particularly when immune suppression is significant.
- 2. Classic: Slower-growing and usually appearing in older adults of Mediterranean or Eastern European descent.
- 3. Endemic: Occurring in parts of Africa, this type affects adults and sometimes children in regions where the virus is more widespread.
- 4. Latrogenic (transplant-associated): Seen in people on long-term immune-suppressing medications after organ transplantation.
Each carries its own pace and considerations, but all share a common viral link at the heart of their development.
Kaposi sarcoma symptoms
These cancer symptoms can be easy to overlook, because they often resemble minor skin or circulation concerns rather than something more significant. All the more reason to be aware of them:
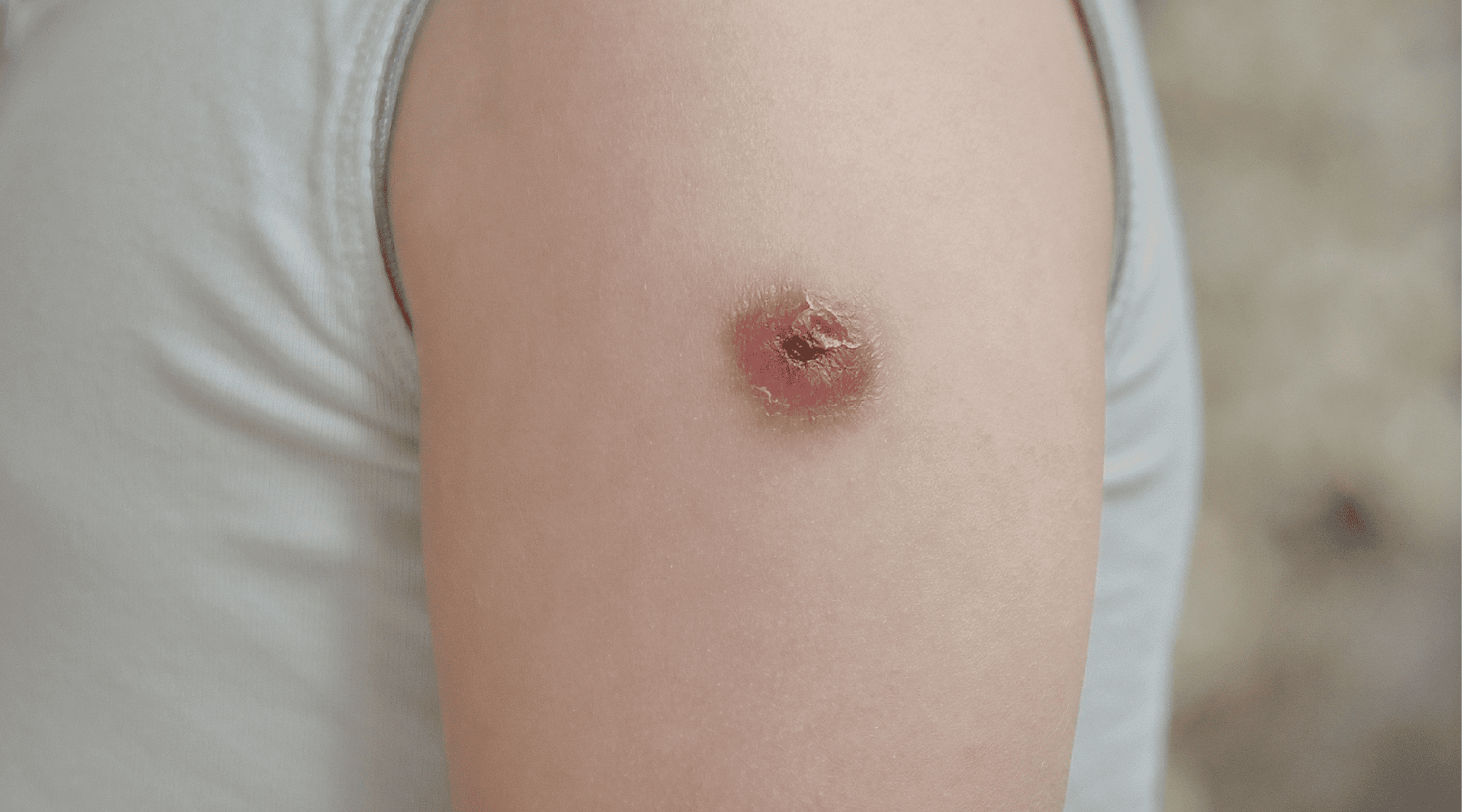
- •Purple, red, or brown patches or bumps on the skin
- •Small clusters or larger areas spreading over time
- •Kaposi sarcoma rash that might be flat or slightly raised
When lesions grow internally, symptoms can reflect the organ involved, such as coughing if the lungs are affected or digestive discomfort if the gastrointestinal tract is involved. The above signs of cancer may be subtle at first and evolve over months or years.
Kaposi sarcoma causes
When we ask “kaposi sarcoma caused by what” factors, the answer centres on both a virus and the state of the immune system.
Role of HHV-8
The kaposi sarcoma virus, known medically as human herpesvirus 8 (HHV-8), plays a central role in the development of this disease.
Infection with HHV-8 is necessary for early kaposi sarcoma to occur, but infection alone does not mean cancer will develop.
Problems arise when the immune system is weakened. When immune defences are low, the virus can become more active, affecting the cells that line blood and lymph vessels.
Over time, persistent immune dysfunction and chronic inflammation may encourage these vascular cells to grow abnormally, leading to tumour formation.
Other risk contributors
Several recognised Kaposi sarcoma risk factors increase the likelihood of developing the disease:
- •HIV infection, particularly when immune suppression is significant
- •Organ transplantation, especially in people taking long-term immune-suppressant medications
- •Men over 60 years of age, particularly those of Mediterranean, Eastern European, or Middle Eastern descent.
- •Living in or originating from sub-Saharan Africa, where HHV-8 infection rates are higher
- •Chronic immune dysfunction, which reduces the body’s ability to control viral activity
These factors do not guarantee disease development, but they help oncology doctors identify who may need closer monitoring.
Kaposi sarcoma diagnostic tests
Accurate cancer diagnostics are essential to distinguish this illness from other skin or vascular conditions that may appear similar. Confirming the diagnosis involves several key steps:
- Biopsy test for cancer: A small sample of a suspicious lesion is removed and examined under a microscope to confirm Kaposi sarcoma.
- Imaging studies: Scans such as X-ray, CT, or endoscopy may be used to check whether lesions involve internal organs.
- Blood tests: Oncologists may assess immune cell counts and viral levels, particularly when Kaposi sarcoma is associated with immune suppression.
These findings are then combined as part of Kaposi sarcoma staging, which determines how far the disease has progressed and helps guide treatment decisions and overall care planning.
Kaposi sarcoma treatment options
The care approach depends on the type, location, and extent of disease, as well as your overall health. It is then shaped into a personalised cancer treatment plan, one that focuses not only on controlling the disease, but also on protecting your quality of life.

Below are some options your oncologist might recommend:
Addressing immune health
For many people, particularly when Kaposi sarcoma is associated with HIV, restoring immune strength can significantly change how the disease behaves. This is done through antiretroviral therapy (ART).
It is a combination of medications that suppress HIV, such as integrase inhibitors (like dolutegravir), nucleoside reverse transcriptase inhibitors (such as tenofovir), and other antiviral agents.
By lowering the HIV viral load and allowing immune cell counts (especially CD4 cells) to recover, ART helps the body regain control over the Kaposi sarcoma herpesvirus. In many cases, this immune recovery alone can slow progression or even cause visible lesions to shrink.
Systemic therapies
When disease is widespread, involves internal organs, or does not improve with immune restoration alone, treatment may involve medications that work throughout the body:
- Chemotherapy: Drugs such as liposomal doxorubicin or paclitaxel are commonly used when lesions are extensive or progressing.
- Immunotherapy: Interferon-alpha may be considered in selected patients with adequate immune function.
- Targeted therapy: Agents such as bevacizumab and sirolimus are being studied and used in specific cases.
Every treatment plan aims to balance effectiveness with daily well-being, often in conversation with your specialists. Early detection of changes, even subtle ones, allows care teams to adapt without unnecessary delay.
Local treatments for skin lesions
When this cancer is limited to small or surface-level lesions, oncologists may recommend targeted local treatments:
- •Radiation therapy:Damaging the cancer cells’ DNA, which shrinks the lesions, reduces bleeding, and relieves pain or swelling.
- •Cryotherapy:Freezing lesions with liquid nitrogen to destroy abnormal cells, often used for small skin spots.
- •Surgical excision:Removal of small, well-defined nodules when they are localized and accessible.
- •Topical treatments:Medications such as imiquimod or retinoid gels applied directly to the skin to reduce lesion growth.
- •Intralesional injection:Injecting chemotherapy agents like vinblastine directly into lesions to shrink them while limiting effects on the rest of the body.
These approaches are typically used when disease is confined to specific areas and do not replace systemic treatment if the cancer is more widespread.
How common and what to expect
Despite how visible it can be, Kaposi sarcoma is relatively rare. Globally, it affects an estimated 30,000–35,000 people each year, with much higher rates in regions where immune-related conditions and viral exposure are more common.
In places like the United States, the condition remains uncommon, with only around 3 to 4 cases per million people each year in the general population. Although rates are higher among people living with HIV.
Survival outcomes vary with spread: if lesions are localised, many people live long lives with treatment; when disease has spread, outcomes can be more serious.
Overall, across stages, kaposi sarcoma survival rate is about 75% for five years after diagnosis, with better outlooks when the disease is caught early and immune health is supported.
Kaposi sarcoma prevention and moving forward
Strengthening Kaposi sarcoma awareness is one of the most practical steps toward prevention. Because this cancer often begins with visible skin changes, recognising early signs and seeking timely evaluation can prevent progression and complications.
For people living with HIV, consistent treatment significantly decreases the likelihood of this cancer developing. For transplant recipients or individuals on immune-modulating medications, regular follow-up allows doctors to adjust therapy when needed.
Prevention is not only about avoiding disease, but also about staying alert to change. When Kaposi sarcoma is identified early, outcomes improve and treatment options remain broader.
Partnering with an experienced oncology centre ensures careful monitoring, informed decisions, and a steady, proactive plan forward.
FAQs
Related Blogs


Recognising the Signs of Cancer in the body that often go unnoticed