What Is Aplastic Anaemia? Symptoms, Cancer Link and Treatment

Most of us rarely give any thought to how our blood quietly does its job every second. But sometimes, subtle changes like unusual tiredness or frequent infections cause concern.
When we hear about rare conditions like aplastic anaemia, we often worry if it’s related to cancer.
Aplastic anaemia refers to a condition where the body stops making enough blood cells. While it’s practically not cancer, it can sometimes be linked to serious bone marrow problems and malignancy.
However, there are ways to diagnose it, manage it, and even treat it effectively.
This guide will walk you through what it really means, how it affects you, and what can be done about it.
What is aplastic anaemia?
Inside our bones, bone marrow contains stem cells that divide to create red blood cells, white blood cells, and platelets. Healthy marrow is dense with these cells.
The aplastic anaemia meaning describes when this production stops. In this condition, stem cells are destroyed or suppressed, and marrow is replaced by fat in a condition called hypocellularity.
This failure causes pancytopenia, where all three blood lines are low.
- Red blood cells carry oxygen. When it’s low, it leads to exhaustion and weakness.
- White blood cells fight infections. When low, infections can become more frequent and harder to fight.
- Platelets help your blood clot. When levels are low (a condition called thrombocytopenia), you may bruise easily or experience unusual bleeding.
The impact of aplastic anaemia is felt throughout your health.
Types of aplastic anaemia
Aplastic anaemia is categorised by its cause and its severity. Identifying the specific types is the primary step in determining the correct medical approach, as treatments for one type may not work for another.
Acquired aplastic anaemia
This is the most common form of aplastic anaemia, particularly in adults. It occurs when a person is born with healthy bone marrow that later fails. It also has a few categories:
- •Idiopathic:In approximately 75% of these cases, the exact trigger is never found. The immune system simply begins to attack the bone marrow's stem cells.
- •Secondary:This type is linked to specific exposures, such as toxic chemicals like benzene, certain medications, or viral infections like hepatitis or Epstein-Barr.
- •PNH-associated:About 40-59% of patients also show signs of Paroxysmal Nocturnal Hemoglobinuria (PNH), a condition where blood cells lack specific protective proteins.
Inherited bone marrow failure syndromes (IBMFS)
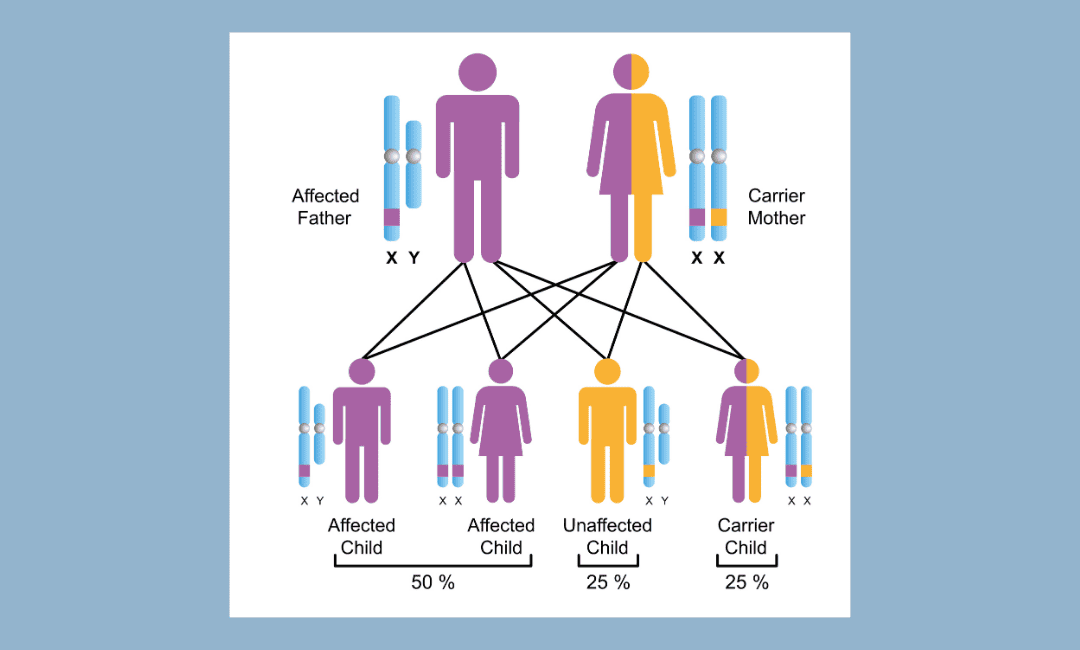
You may ask, is aplastic anaemia genetic? In some instances, it is. These syndromes are caused by gene mutations passed from parents to children.
They are typically diagnosed in childhood and often include physical signs like short stature or skin changes.
Common types of this kind of aplastic anaemia are Fanconi Anaemia and Dyskeratosis Congenita.
Aplastic anaemia symptoms & causes
Your body usually sends both clear and ambiguous signals when it is struggling. Because aplastic anaemia affects all three types of blood cells, the signs of aplastic anaemia appear in three different ways.
Recognizing the symptoms
When your bone marrow fails to produce cells, your body reacts to the specific shortage:
- •Low red blood cells:This leads to a lack of oxygen in your tissues. You may feel constant fatigue, have pale skin, or experience shortness of breath.
- •Low white blood cells:These cells are your defence system. Without them, you might notice frequent infections that take a long time to heal, or you may develop fevers and chills for no clear reason.
- •Low platelets:Platelets help your blood clot. Low levels lead to symptoms like easy bruising, tiny red spots on the skin (petechiae), frequent nosebleeds, or bleeding gums.
Understanding the causes
But why would the immune system suddenly turn against the bone marrow? While most cases are of unknown origin, there are several identified aplastic anaemia causes.
- •Environmental toxins:Long-term exposure to chemicals like benzene (found in gasoline and some paints) or certain pesticides can damage stem cells.
- •Medical treatments:High-dose radiation or chemotherapy used for cancers can sometimes accidentally damage healthy marrow cells.
- •Viral triggers:Certain viruses, such as hepatitis or the Epstein-Barr virus, can trigger an immune response that mistakenly attacks the marrow.
- •Autoimmune shifts:Sometimes the body's own T cells, which normally fight disease, begin to see the bone marrow as a threat. This can also happen during pregnancy when the immune system undergoes complex changes.
By identifying the aplastic anaemia etiology, pathologists and oncologists (if you’re going through cancer care) can better understand how the condition started and how to stop its progression.
Aplastic anaemia grading and classification
We use grading to decide how quickly you may need treatment. The aplastic anaemia diagnosis criteria allow medical teams to measure bone marrow failure and choose the right level of care.
| Severity level | Aplastic anaemia criteria |
|---|---|
| Non-severe (moderate) | The bone marrow is less than 25% active, but blood counts have not yet reached the critical thresholds for severe disease. |
| Severe aplastic anaemia (SAA) | The bone marrow is less than 25% active, and at least two blood cell lines (red, white, or platelets) are critically low. |
| Very severe (vSAA) | Same as severe, but the white blood cell count (neutrophils) is under 200/µL, creating an immediate risk of infection. |
This aplastic anaemia classification is essential because it identifies who needs an urgent transplant or intensive medication, as in some cases, lymphoma is also a possibility.
Specifically, an extremely low neutrophil count is the strongest predictor of how well a patient will survive the initial phase of the disease.
Cancer link and risk factors
While the answer to is aplastic anaemia cancer is no, a connection exists because marrow stress can cause surviving cells to change. This evolution may lead to blood cancers like MDS or AML in 10-15% of acquired cases over ten years.
| Risk factor | Impact on aplastic anaemia prognosis |
|---|---|
| Disease duration | The longer the marrow is inactive, the more stress is placed on cells, increasing mutation risks. |
| Genetic changes | Losing parts of genetic code, such as chromosome 7, significantly raises cancer risk factors. |
| Specific mutations | Some mutations (PIGA) help recovery, while others (ASXL1) are linked to a higher risk of leukemia. |
| Long-term care | Regular monitoring is essential to catch aplastic anaemia complications like MDS early. |
Aplastic anaemia diagnosis
Diagnostics usually moves from simple blood tests to a more detailed review of your bone marrow.
| Test name | What it tells us |
|---|---|
| Complete blood count (CBC) | Measures red cells, white cells, and platelets; all three are typically low in this condition. |
| Reticulocyte count | Counts young red blood cells; a low number proves the marrow is not producing new cells. |
| FNAC test | FNAC test is sometimes used to examine cell patterns or rule out other conditions like lymphoma. |
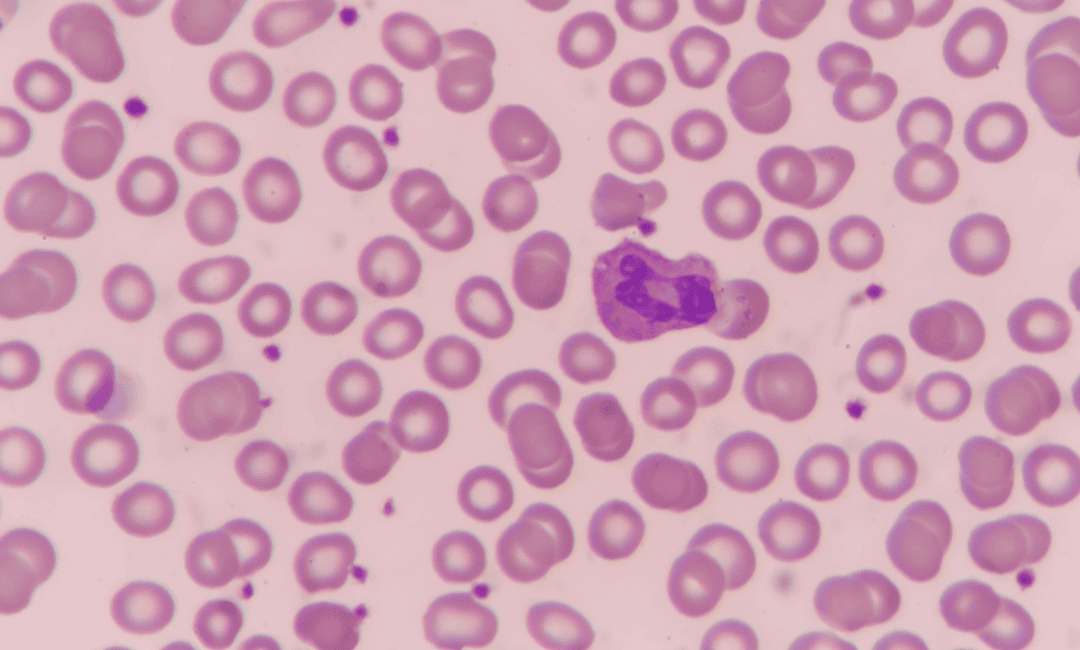
| Peripheral blood smear | This confirms if the cells look normal and rules out abnormal "blast" cells found in leukaemia. |
| Bone marrow biopsy | Biopsy test for cancer shows if the marrow is "empty" and confirms that the low counts are not caused by an overgrowth of cancer cells. |
| Cytogenetics | Looks for chromosomal changes, like the loss of chromosome 7, which could increase the risk of developing blood cancer later. |
| Flow cytometry | Screens for PNH, a related condition where cells lack specific proteins that protect them from the immune system. |
By ruling out what causes cancer and other diseases, your medical team can focus entirely on the best way to support and heal your bone marrow.
Aplastic anaemia treatment and management
Treatment aims to restart blood production. If your immune system attacks the marrow, we must stop the attack or replace the system. Many ask: is aplastic anaemia curable? For many, the answer is yes.
Supportive care
Management of aplastic anaemia begins with safety. Because your marrow is quiet, doctors use red cell and platelet transfusions to keep you stable. Protective medicines also help prevent infections while white cell counts are low.
The three-drug path
If a transplant is not an option, a three-drug plan is common:
- •ATG:A hospital medicine that stops immune cells from attacking marrow.
- •Cyclosporine:A pill that keeps the immune system calm.
- •Eltrombopag:A drug that helps stem cells grow. Generic versions now help lower the aplastic anaemia treatment cost.
Bone marrow transplant
A transplant is often best for younger patients with a matched sibling. By using healthy donor cells, the aplastic anaemia cure rate can reach 80% to 90%.
Even without a sibling match, half-match transplants are now also very successful if you have a cancer diagnostics.
Prevention and pregnancy
There is no certain aplastic anaemia prevention for the autoimmune type, but avoiding chemicals like benzene reduces risk for the acquired type.
For women, pregnancy requires a specialist team to keep mother and baby safe from aplastic anaemia side effects.
Next step forward
It’s a serious marrow condition, but modern therapy and transplants now offer high aplastic anaemia survival rate. Understanding the signs and securing prompt cancer screening tests are the first vital steps toward healing and regaining your physical health.
Everhope Oncology supports this path with specialized diagnostics and personalized cancer treatment. Our team uses advanced therapies to manage bone marrow failure effectively and provides the guidance you need to confidently move toward healing.
FAQs
Related Blogs

The Role of Oxidative Stress in Cancer: A Guide to Your Cellular Health